How Digital Dentistry Is Changing the Patient Experience
Dentistry has changed more in the last 10 years than in the previous 50.
Thanks to digital technology, modern dental care is now faster, more precise, and more predictable than ever before.
Dentistry has quietly gone through a technology revolution over the last decade. While many people still imagine dental care as impressions, molds, and long waiting periods, modern practices are increasingly powered by advanced digital tools that allow treatment to be faster, more accurate, and far more predictable.
This shift is not just about new machines — it is about a better experience for patients.
From 3D scanning and virtual treatment planning to same-day teeth and guided implant surgery, digital dentistry is transforming how dental care is delivered. And for patients, that means fewer appointments, clearer explanations, and greater confidence in outcomes.
Let’s explore what digital dentistry really means, how it works, and why it matters to you.
What Is Digital Dentistry?
Digital dentistry refers to the use of advanced imaging, scanning, and computer-based design to plan and deliver dental treatment.
Instead of relying on:
physical molds
stone models
guesswork during surgery
long lab turnaround times
Digital dentistry uses:
3D scans of your teeth and jaw
Digital treatment simulations
Computer-guided implant placement
On-site fabrication of dental restorations
In modern digital practices, your entire treatment — from diagnosis to final result — can be designed virtually before anything is done in your mouth.
This creates a level of precision and predictability that simply was not possible in traditional dentistry.
The Old Way vs the Digital Way
Traditional Dentistry
Physical impressions that could be uncomfortable
Two to three weeks waiting for crowns or prosthetics
Limited visualization of outcomes
More manual adjustments
Higher chance of remakes
Digital Dentistry
Small 3D scanners instead of impression trays
Digital models instead of stone casts
Virtual simulations of your final smile
Computer-guided implant placement
Faster turnaround and fewer visits
For patients, this often means:
Less gagging
Shorter appointments
Fewer surprises
Better-fitting restorations
More confidence in treatment decisions
Seeing Before Doing: Why Visualization Matters
One of the most important changes digital dentistry brings is the ability to see your treatment before it happens.
Instead of trying to imagine what your dentist is describing, you can now view:
a 3D model of your teeth
your bone structure
your bite
your future smile design
This helps answer common patient questions:
What will my teeth look like?
Where will the implants go?
How much bone do I have?
Will this work for me?
When patients can see their condition and the proposed solution, they tend to feel:
more informed
more confident
less anxious
more involved in decision-making
Dentistry becomes collaborative instead of mysterious.
Digital Dentistry and Dental Implants
Dental implants benefit more from digital technology than almost any other area of dentistry.
In traditional implant surgery, placement was largely guided by experience and judgment at the time of surgery. While this worked well for many years, it left more room for variation.
With digital dentistry:
your jaw is scanned in 3D
implant positions are planned virtually
nerves and sinuses are mapped
bite forces are considered
a surgical guide can be fabricated
This allows implants to be placed with:
greater precision
improved safety
better long-term stability
more predictable esthetic results
For patients, this often translates to:
less surgical trauma
reduced swelling
faster healing
more confidence in the final outcome
Same-Day and Accelerated Dentistry
One of the most noticeable changes for patients is how much faster treatment can be.
With traditional methods:
crowns often took weeks
dentures required multiple visits
implant restorations could take months
With digital workflows:
teeth can be designed digitally
restorations can be fabricated in-office
treatment timelines can be compressed
In some cases, this allows for:
same-day crowns
immediate implant teeth
fewer overall appointments
This is especially valuable for patients who:
travel
work full-time
have dental anxiety
want faster solutions
Speed is not just convenience — it reduces disruption to daily life.
Comfort: Less Mess, Less Guessing
Many patients’ least favorite part of dentistry is traditional impressions.
Digital scanning replaces messy materials with a small handheld camera that captures thousands of images per second. These images are stitched together into a precise 3D model of your teeth.
Benefits include:
no gagging
no bad taste
higher accuracy
immediate feedback
Digital scanning also allows:
easier retakes if needed
real-time verification
better fit of restorations
Better data leads to better results.
Why Some Practices Are Farther Ahead Than Others
Not all digital dentistry is equal.
Some practices:
scan but still send everything out
use digital tools only for certain cases
rely heavily on external labs
More advanced digital practices:
design restorations in-house
use 3D imaging routinely
plan implant surgery virtually
fabricate guides and models on-site
When a practice controls the entire digital process, it means:
less outsourcing
faster turnaround
more customization
tighter quality control
This is similar to the difference between:
ordering something online
vshaving it custom-built locally
The more of the process that happens under one roof, the more predictable the result can be.
How Technology Improves Safety
Digital dentistry improves safety by allowing dentists to:
map nerves and sinuses
plan implant depth and angle
avoid critical structures
simulate surgery beforehand
This reduces:
guesswork
unnecessary bone removal
risk of complications
chance of needing revisions
In complex cases such as full-arch implant treatment, digital planning can be the difference between:
a carefully engineered result
anda purely manual one
Patients benefit from:
greater precision
fewer surprises
clearer expectations
What This Means for Patients Considering Big Treatment
For patients facing:
dental implants
full-arch tooth replacement
cosmetic smile changes
complex restorations
Digital dentistry provides:
visual previews
predictable planning
customized design
better communication
Instead of asking, “Will this work?”
patients can now ask, “Does this plan make sense to me?”
That is a major shift in how dental decisions are made.
Trust, Transparency, and Confidence
Modern patients expect:
clarity
transparency
modern tools
efficient care
Just like medicine, banking, and travel, dentistry is becoming more digital because expectations have changed.
Patients want:
fewer visits
faster answers
clear explanations
modern solutions
Digital dentistry supports this by making treatment:
more understandable
more visual
more predictable
It also helps patients feel that their care is:
carefully planned
customized
based on real data
Not guesswork.
The Future of Dentistry Is Digital
Digital dentistry is not a trend — it is a permanent shift in how care is delivered.
As technology continues to evolve, patients can expect:
more customization
shorter timelines
more precise treatment
more comfortable experiences
Practices that fully embrace digital systems are not just using new tools — they are redesigning the way dentistry works.
For patients, this means dentistry is becoming:
more human
more understandable
more efficient
more reliable
Why This Matters When Choosing a Dental Practice
When choosing a dentist, it is reasonable to ask:
Do they use digital scanning?
Do they plan treatment virtually?
Do they use 3D imaging for implants?
Do they design and fabricate restorations digitally?
These questions are not about gadgets.
They are about:
precision
predictability
patient experience
quality control
A digitally advanced practice can often:
reduce treatment time
increase comfort
improve long-term outcomes
Final Thoughts
Digital dentistry has transformed what is possible in modern dental care.
By combining:
3D imaging
digital design
computer-guided treatment
on-site fabrication
Dentists can now plan your care before it begins and execute it with unprecedented accuracy.
For patients, this means:
clearer understanding
fewer surprises
faster results
greater confidence
Dentistry is no longer just about fixing teeth.
It is about engineering solutions — with your comfort, safety, and outcome in mind.
And that is what truly modern dental care looks like.
Prosthodontist vs. General Dentist: Who Should Do Full-Mouth and Implant Cases?
Learn the difference between a prosthodontist and a general dentist for full-mouth reconstruction and dental implants, and which is right for complex cases.
If you’ve been told you need extensive dental treatment — such as dental implants, full-mouth reconstruction, or replacement of many teeth — you may wonder:
Should I see a general dentist or a prosthodontist?
And what is the difference between them?
Many dental offices advertise “full-mouth restoration” or “implant dentistry,” but not all providers have the same training or focus. Understanding these differences can help you make a more confident decision about your care.
What Does a General Dentist Do?
A general dentist is similar to a family doctor for your teeth. They provide routine dental care such as:
Cleanings and exams
Fillings and crowns
Basic cosmetic dentistry
Preventive care
Simple tooth extractions
Some general dentists also take advanced continuing education in implants and complex dental treatments. They may market themselves as “full-mouth” or “implant-focused” dentists.
This can be appropriate for certain patients and certain cases — but large or complex reconstructions involve additional planning, risks, and long-term considerations.
What Is a Prosthodontist?
A prosthodontist is a dental specialist who completes:
Four years of dental school
Plus three additional years of advanced specialty training in complex tooth and implant restoration
Prosthodontists are trained specifically in:
Full-mouth reconstruction
Dental implants and implant-supported teeth
Bite alignment and jaw function
Esthetic smile design
Failing crowns, bridges, and implants
Coordinating care with oral surgeons and periodontists
In simple terms:
A prosthodontist specializes in rebuilding smiles when dental problems are complex or extensive.
The Biggest Difference: Planning the Outcome
One of the most important differences between a prosthodontist and a general dentist is how treatment is planned.
General dentists often focus on performing individual procedures.
Prosthodontists focus on:
Designing how the final teeth should look and function
Planning where implants should be placed before surgery
Coordinating surgical and restorative steps
Managing the bite, facial support, and long-term durability
This type of planning is critical for:
Full-arch dental implants
“All-on-X” implant treatments
Severe tooth wear or bite collapse
Patients with bone loss or gum disease
Replacing many missing teeth
Correcting failed dental work
When many teeth are involved, small mistakes in planning can affect comfort, appearance, and long-term success.
Why Does This Matter for Patients?
Full-mouth and implant cases involve more than replacing teeth. They involve:
Tooth position
Bite height
Implant angles
Gum support
Smile design
Material selection
These decisions influence:
How natural your smile looks
How long your restorations last
How easy your teeth are to clean
How comfortable your bite feels
The risk of future complications
Complex cases benefit from a provider whose primary focus is designing and restoring entire dental systems — not just treating one tooth at a time.
Why Do Some General Dentists Offer Full-Mouth Treatment?
Some general dentists pursue extensive training and enjoy providing comprehensive care. Others work closely with specialists to co-manage larger cases.
However, many general dentists choose to refer complex cases because:
They are higher risk
They require detailed planning
They involve long treatment timelines
They can be emotionally and financially stressful for patients
Referring a patient to a prosthodontist is often a decision made in the patient’s best interest — not because the dentist lacks ability, but because the case requires specialized focus.
When Should You Consider Seeing a Prosthodontist?
You may benefit from seeing a prosthodontist if you:
Need full-mouth reconstruction
Are missing many teeth
Need multiple dental implants
Have worn, broken, or collapsing teeth
Have failed crowns, bridges, or implants
Have gum disease with bite problems
Want a second opinion before major dental treatment
Have been unhappy with previous dental work
Want a long-term, carefully planned solution
Many patients seek a prosthodontist after visiting an implant center or a general dentist who advertises full-mouth care — especially when they want a more detailed explanation of their options.
Prosthodontist vs. Implant Center: Is There a Difference?
Implant centers often focus on:
Speed
One-location treatment
High-volume implant placement
A prosthodontist focuses on:
Long-term function
Bite and esthetics
Planning before surgery
Coordinating care between providers
Managing complications
For patients who want predictable, long-lasting results — especially for complex cases — treatment planning can be just as important as the surgery itself.
Which Is Better: General Dentist or Prosthodontist?
There is no single “better” choice for every patient.
For routine dental care, a general dentist is usually the right provider.
For simple implant cases, a trained general dentist may be appropriate.
For complex or full-mouth cases, a prosthodontist offers specialized training in reconstruction and planning.
The most important factor is matching:
the complexity of the problem
with the experience and training of the provider.
Final Thoughts
If you are facing major dental treatment, you deserve:
A clear and thorough plan
Honest discussion of risks and alternatives
A provider who regularly treats complex cases
A long-term perspective, not just a quick fix
Whether your care involves a general dentist, a surgeon, and a prosthodontist working together — or is coordinated within one office — the goal should always be a result that looks natural, functions well, and lasts.
If you have been told you need extensive dental work and would like a second opinion, consulting with a prosthodontist can help you better understand your options before making a decision.
Do Dental Implants Need Healthy Gums? The Role of Keratinized Tissue Explained
Most patients focus on the implant itself—but the health of your gum tissue plays a critical role in long-term success. Keratinized tissue, the firm protective gum around your implant, helps prevent discomfort, supports easier cleaning, and reduces the risk of complications. In this article, we break down why this often-overlooked factor can make all the difference in how your implant looks, feels, and lasts.
When people think about dental implants, they usually focus on the visible result—the new tooth. But one of the most important factors for long-term success often goes unnoticed: the health of the gum tissue surrounding the implant, especially something called keratinized tissue.
This type of tissue plays a critical role in comfort, hygiene, and the longevity of your implant. Understanding why it matters can help you protect your investment and maintain a healthy, confident smile for years to come.
What Is Keratinized Tissue?
Keratinized tissue is the firm, dense, and slightly “tougher” gum tissue that surrounds your teeth—and ideally, your dental implants. It’s the pale pink gum you see when you look in the mirror, as opposed to the darker, more movable tissue found deeper in your mouth.
This tissue contains keratin, a protective protein that also exists in your skin, hair, and nails. Its job is to create a strong, resilient barrier that can withstand the daily stresses of chewing, brushing, and bacteria.
Around natural teeth, keratinized tissue forms a stable seal. Around dental implants, it serves a very similar purpose—but its role can be even more important.
Why Does Keratinized Tissue Matter Around Implants?
Unlike natural teeth, dental implants don’t have a periodontal ligament—a cushion-like structure that helps protect and support real teeth. Because of this, implants rely more heavily on the surrounding bone and soft tissue for stability and defense.
That’s where keratinized tissue becomes essential.
1. It Creates a Protective Barrier
Keratinized tissue acts as a shield against bacteria. When there is enough of it around an implant, it helps prevent inflammation and infection by forming a tighter, more stable seal.
Without this protective barrier, bacteria can more easily penetrate the tissue and reach the bone that supports the implant.
2. It Improves Comfort
Patients with little or no keratinized tissue around their implants often report discomfort when brushing or eating. The softer, non-keratinized tissue is more sensitive and prone to irritation.
When brushing is uncomfortable, people naturally avoid it—and that can lead to plaque buildup and long-term problems.
With adequate keratinized tissue, daily hygiene feels easier and more comfortable, making it more likely that you’ll maintain a healthy routine.
3. It Supports Better Oral Hygiene
Healthy implants depend on consistent, effective cleaning. Keratinized tissue provides a stable, non-movable surface that makes brushing and flossing more efficient.
When the tissue is thin or mobile, it can be difficult to clean thoroughly without causing irritation. Over time, this can increase the risk of inflammation around the implant.
4. It Reduces the Risk of Peri-Implant Disease
One of the biggest concerns with dental implants is a condition called Peri-implantitis—an infection that affects the gum and bone surrounding an implant.
Peri-implantitis can lead to bone loss and, in severe cases, implant failure.
Studies have shown that implants surrounded by adequate keratinized tissue tend to have lower rates of inflammation and are easier for patients to keep clean. While it’s not the only factor, it plays a meaningful role in reducing risk.
5. It Enhances Long-Term Stability
Dental implants are designed to last for many years, even decades. But their success depends on the health of the surrounding environment.
Keratinized tissue helps maintain stable gum levels and protects against recession (when the gum pulls away from the implant). This is especially important in visible areas of the smile, where even slight changes can affect appearance.
What Happens If There Isn’t Enough Keratinized Tissue?
Not every patient naturally has an ideal amount of keratinized tissue—especially in areas where teeth have been missing for a long time.
If there isn’t enough, you may experience:
Gum sensitivity or soreness
Difficulty brushing comfortably
Increased plaque buildup
Inflammation or bleeding around the implant
A higher risk of long-term complications
It’s important to understand that an implant can still function in these situations—but it may require more maintenance, closer monitoring, and sometimes additional treatment to ensure long-term success.
Can Keratinized Tissue Be Improved?
Yes—and this is one of the most important parts of modern implant care.
If your dentist or specialist determines that there isn’t enough keratinized tissue, they may recommend a soft tissue grafting procedure. This involves adding tissue to strengthen and stabilize the area around the implant.
These procedures are commonly performed and can make a significant difference in both comfort and long-term outcomes.
In some cases, this is done before implant placement to prepare the site. In others, it may be recommended after the implant is placed if symptoms or concerns arise.
How Do You Know If You Have Enough?
This isn’t something you can easily measure at home, but there are signs that may indicate a problem:
Discomfort when brushing near your implant
Gums that look thin, shiny, or mobile
Persistent redness or inflammation
Bleeding when cleaning around the implant
The best way to evaluate this is through a professional exam. Your dental provider will assess the thickness, width, and quality of the tissue and determine whether any intervention is needed.
What You Can Do to Protect Your Implant
Even with ideal keratinized tissue, daily care plays a major role in implant success. Here are a few simple but powerful steps you can take:
Brush gently but thoroughly around your implant twice a day
Use floss or specialized implant cleaning tools to remove plaque
Attend regular dental visits for professional cleanings and monitoring
Report any discomfort or changes early, before they become bigger issues
Think of your implant like a high-performance investment—it performs best when it’s properly maintained.
The Bigger Picture: It’s Not Just About the Tooth
Dental implants are one of the most advanced and reliable solutions in modern dentistry. But their success isn’t just about placing a titanium post in the bone—it’s about creating a healthy, balanced environment around it.
Keratinized tissue is a key part of that environment.
While it may seem like a small detail, it can make a big difference in how your implant feels, functions, and lasts over time.
Final Thoughts
If you’re considering dental implants—or already have them—it’s worth having a conversation about the health of your gum tissue.
A beautiful result is important, but so is long-term comfort and stability.
By paying attention to factors like keratinized tissue, you’re not just restoring your smile—you’re protecting it for the future.
If you have questions about your implants or want to learn more about optimizing your results, scheduling a consultation is the best place to start. Your smile deserves that level of care.
Implant Centers vs. Comprehensive Dental Care: What’s the Difference?
Learn the difference between implant centers and comprehensive dental care in New Hampshire and how each approach affects long-term results.
If you’ve been researching dental implants or full-arch tooth replacement, you’ve probably seen ads for large implant centers promising fast results and “teeth in a day.” You may also have heard your dentist talk about a more comprehensive approach to care.
To patients, these options can sound similar — but they are built on very different philosophies.
Understanding the difference can help you choose the type of care that’s right for you, especially for complex treatments like full-arch dental implants.
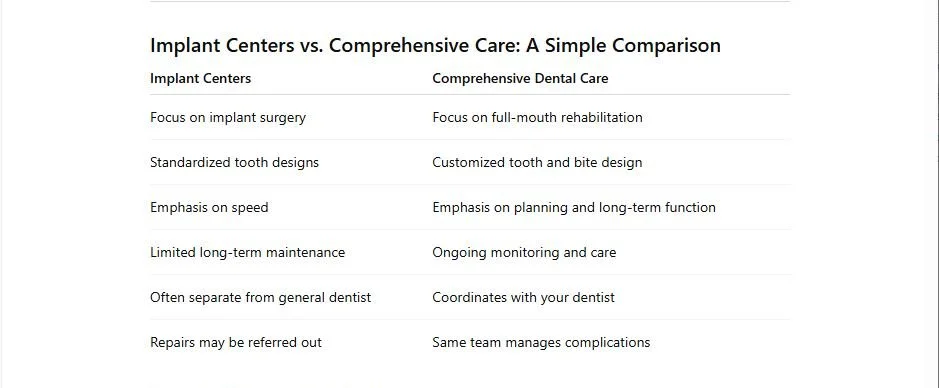
Two Different Models of Care
Implant Centers: Procedure-Focused Care
Implant centers are typically designed around one main service: placing dental implants. Their model is built for efficiency and volume.
They often emphasize:
• speed
• convenience
• same-day teeth
• set treatment packages
• centralized scheduling
• advertising-based patient flow
Their primary focus is the surgical procedure itself.
This can be appealing to patients who want a fast, simplified process.
Comprehensive Dental Care: Health-Focused Rehabilitation
A comprehensive dental practice looks at your mouth as a complete system — not just where implants can be placed.
This model emphasizes:
• long-term function
• bite balance
• aesthetics
• speech
• hygiene access
• maintenance
• coordination with your general dentist
The primary focus is the final result and how it holds up over time, not just the day of surgery.
Why This Difference Matters
Dental implants don’t work in isolation. They support teeth that must function every day when you eat, speak, and smile.
Long-term success depends on:
• how the teeth are designed
• how your bite fits together
• how forces are distributed
• how easy the restoration is to clean
• how your jaw joints respond
• how the materials wear over time
If treatment focuses only on placing implants, these factors can be overlooked or simplified.
A comprehensive approach plans the teeth first, then places the implants to support that plan.
Both models can place implants. The difference is what happens before surgery — and after it.
Common Questions Patients Ask
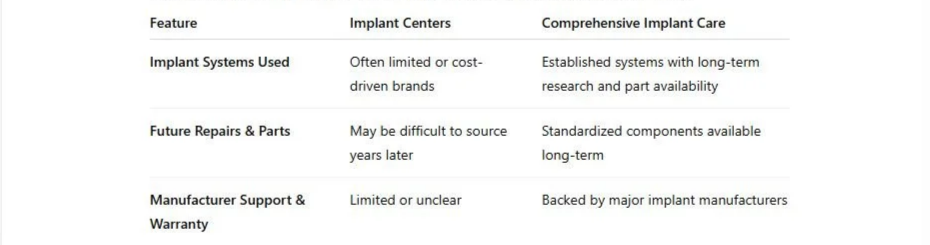
“Aren’t all dental implants the same?”
Many patients assume that all dental implants are the same — but just like cars or medical devices, implant systems vary widely in quality, support, and long-term reliability.
Some offices use lesser-known or private-label implant brands that may cost less upfront. While these implants can work in certain situations, they often come with important limitations:
Limited long-term research data
Fewer restorative component options
Difficulty finding replacement parts years later
Little or no manufacturer warranty
Less technical and clinical support for complex cases
By contrast, well-established implant systems from major manufacturers — such as Nobel Biocare — are backed by decades of clinical research, global availability, and strong restorative compatibility. This matters because dental implants are meant to last for decades, not just years.
If an implant or prosthesis ever breaks, loosens, or needs repair, access to standardized components and manufacturer support can make the difference between a simple fix and a complete redo.
“Why do prices vary so much?”
Lower-cost options often focus on:
• standardized prosthetics
• limited customization
• minimal follow-up
• fewer long-term services
More comprehensive care usually includes:
• detailed planning
• customized design
• multiple try-ins or prototypes
• long-term monitoring
• management of complications
• coordination with your dentist
The true cost of treatment is not just the initial price — it’s what happens if something breaks, wears out, or becomes uncomfortable later.
“Is one safer than the other?”
Both models can place implants successfully.
The difference is what happens:
• before surgery
• after surgery
• years later
Comprehensive care places more emphasis on:
• prevention of complications
• early detection of problems
• maintenance
• long-term stability
This can reduce the likelihood of needing major repairs later.
What Happens If Something Goes Wrong?
This is an important question many patients don’t think to ask.
With procedure-focused models:
• you may be referred elsewhere for repairs
• ongoing care may not be included
• responsibility may be divided between offices
With comprehensive care:
• the same team usually manages
– your implants
– your teeth
– your bite
– your long-term maintenance
This continuity can be important if adjustments or corrections are needed. For patients, the real question is not just “Can I get implants?” but:
“Will my implants still be serviceable 10 or 20 years from now?”
Choosing a provider who uses proven implant systems and plans for long-term maintenance can reduce the risk of future complications, costly replacements, and unexpected failures.
This is one of the reasons comprehensive implant practices focus not just on placing implants — but on designing restorations that can be repaired, upgraded, and maintained over time.
How Treatment Philosophy Affects Your Experience
In a Procedure-Focused Model:
You may experience:
• faster treatment
• fewer appointments
• standardized designs
• less customization
• limited long-term follow-up
In a Comprehensive Care Model:
You may experience:
• more planning appointments
• more discussion
• test phases for comfort and appearance
• adjustments over time
• ongoing maintenance visits
Neither is automatically “right” or “wrong.”
They simply serve different patient needs and expectations.
Which Approach Is Right for You?
Implant centers may be a fit if you:
• want the fastest possible process
• are comfortable with standardized solutions
• prefer a surgical-only focus
• do not need complex bite correction
• plan to manage long-term care elsewhere
Comprehensive care may be a better fit if you:
• want customized teeth
• care about long-term function
• have a history of dental problems
• grind or clench
• want one team managing everything
• value ongoing support
• want help if complications occur
Questions to Ask Any Provider
Before choosing where to have implant treatment, ask:
• Who designs my teeth?
• How is my bite planned?
• What materials will be used?
• How will my speech and comfort be evaluated?
• Who manages long-term maintenance?
• What happens if something breaks?
• Who do I call if I have a problem in 5 years?
The answers matter more than the brand name of the implants or how fast the surgery is done.
Our Philosophy
We believe replacing teeth should be treated as a long-term rehabilitation — not just a procedure.
That means:
• planning the final teeth first
• placing implants to support that plan
• designing for comfort, speech, and cleaning
• monitoring results over time
• helping patients if problems arise
Some patients come to us for their first implant treatment.
Others come because something didn’t work elsewhere.
Both deserve careful planning and honest guidance.
The Bottom Line
Implant centers and comprehensive dental practices approach tooth replacement differently.
One focuses primarily on placing implants.
The other focuses on rebuilding how your mouth functions over time.
If you are considering dental implants — especially full-arch treatment — take time to understand which model aligns with your goals, expectations, and comfort level.
Your smile is not just a procedure.
It’s part of your daily life.
And how it’s designed matters.
Why Full-Arch Dental Implants Sometimes Fail — and How an Experienced Team Can Fix Them
Learn why full-arch dental implants can fail, common complications, and how experienced dental teams correct and prevent problems long-term.
Full-arch dental implants (often called “All-on-4” or “teeth in a day”) have transformed dentistry. For many people who have struggled with loose dentures or failing teeth, this treatment can restore the ability to eat comfortably, speak clearly, and smile with confidence.
When done properly, full-arch treatment can be life-changing.
But it is also one of the most complex procedures in dentistry. And like any complex medical treatment, complications can occur.
Some patients come to us after treatment elsewhere and say:
“My teeth keep breaking.”
“My bite feels off.”
“I was told this would last forever.”
“I’m embarrassed to smile.”
“I don’t know who to go to anymore.”
These patients often feel frustrated, confused, or even ashamed — as if they did something wrong.
In most cases, they didn’t.
Full-arch treatment is not just about placing implants. It is a long-term dental rehabilitation involving surgery, prosthetics, bite design, materials, and maintenance. When any part of that system is overlooked, problems can develop months or years later.
This article explains:
• why full-arch complications happen
• what warning signs to look for
• and how experienced teams correct and prevent these problems
Our goal is not to criticize other providers. It is to help patients understand what truly determines long-term success.
Full-Arch Treatment Is a System, Not a Single Procedure
Many people assume full-arch treatment is mainly about surgery. In reality, implant placement is only the foundation.
The teeth that attach to the implants must:
fit passively without strain
distribute biting forces evenly
support natural speech
look proportionate to the face
allow proper cleaning
resist wear and fracture
protect the implants from overload
Clinical studies consistently show that long-term success depends not only on implant survival, but on prosthetic design, occlusion (bite), and hygiene access.
In simple terms:
The implants hold the teeth — but the teeth determine whether the implants last.
This is why planning must start with the final teeth, not just with where implants can be placed in bone.
Common Problems Seen in Struggling or Failed Full-Arch Cases
1. Fractured or Worn Teeth
One of the most common complications is broken or severely worn prosthetic teeth.
Contributing factors include:
heavy bite forces or grinding
imbalanced occlusion
thin prosthetic materials
insufficient implant support
lack of night protection
Acrylic and composite teeth, which are often used in provisional or economy restorations, are known to wear faster under heavy forces. Even stronger materials can fail if the bite is not designed properly.
Patients often assume breakage is unavoidable. In reality, repeated fractures usually point to a design or bite problem rather than simple bad luck.
2. Bite Problems and Jaw Discomfort
A full-arch restoration must distribute chewing forces evenly across implants and jaw joints.
When it does not:
implants may loosen
screws can fracture
jaw muscles fatigue
headaches may develop
chewing feels strained
These problems often appear gradually, not immediately after surgery. Over time, the muscles and joints compensate for an imbalanced bite until symptoms develop.
3. Speech and Aesthetic Concerns
The position and thickness of prosthetic teeth strongly affect speech and facial appearance.
Improper design may lead to:
lisping or whistling
bulky or unnatural contours
food trapping
lip distortion
poor facial support
Speech problems are rarely caused by the implants themselves. They are usually caused by tooth position and prosthetic shape.
4. Hygiene Difficulties and Inflammation
Studies show that long-term implant health depends heavily on plaque control.
If a prosthesis is difficult to clean:
inflammation can develop
odor and bad taste may occur
bone loss can follow
infections may develop
Many patients are told simply to “use a Waterpik,” without individualized instruction or professional maintenance. Design and hygiene education are equally important.
5. Implant Loss
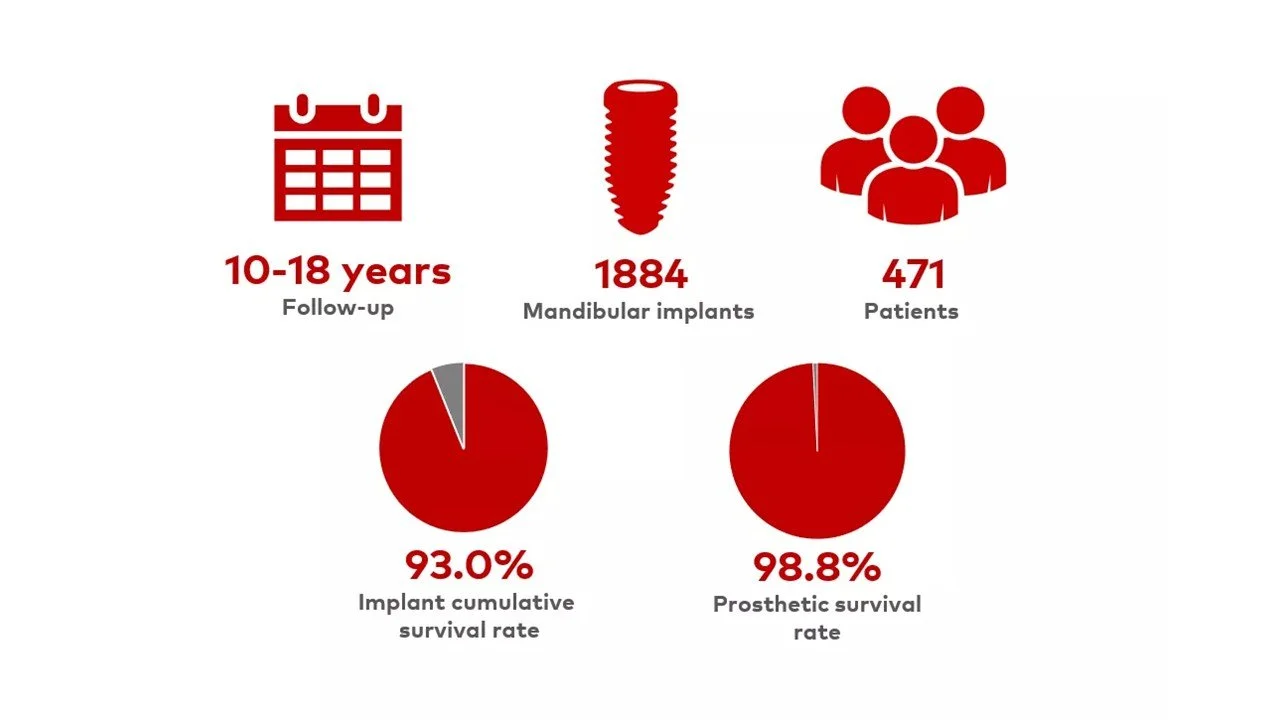
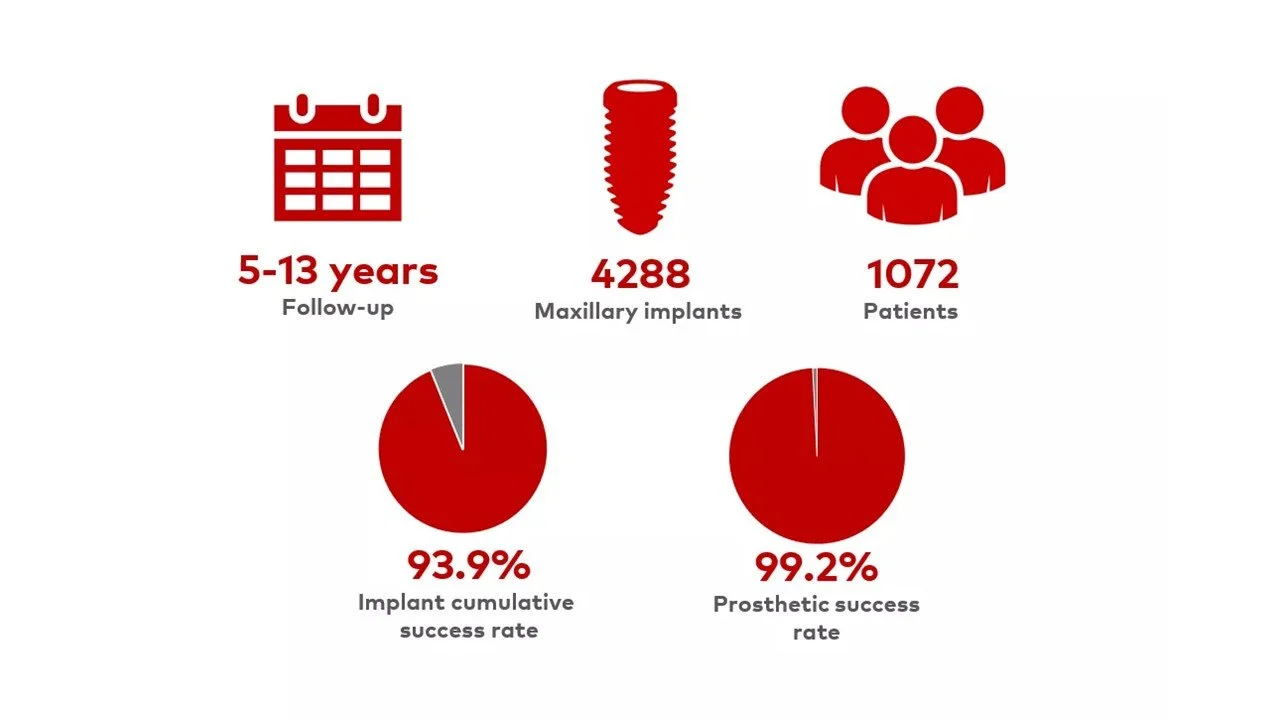
Reported long-term implant survival rates for full-arch treatment are generally high (often above 90% over 5–10 years in controlled studies), but failures do occur.
Implant loss is more commonly associated with:
overload from poor bite design
untreated inflammation
smoking
uncontrolled diabetes
poor oral hygiene
prosthetic misfit
When implants fail, patients experience both emotional distress and financial burden — especially if they believed the solution was permanent.
Why These Problems Occur
Most complications arise from one or more of the following:
1. Surgery-First Planning
In some treatment models, implants are placed first and teeth are designed afterward.
This approach can work, but it increases risk if prosthetic design is not carefully planned in advance. When implants are placed without regard to the final tooth position, the prosthesis must adapt — sometimes poorly.
Prosthetic-driven planning reduces the need for compromise.
2. Standardized Prosthetic Designs
Every patient has different:
facial proportions
muscle strength
jaw shape
bite pattern
speech dynamics
Standardized arches save time, but they reduce customization. What works well for one patient may be inappropriate for another.
Long-term success depends on individualized design.
3. Lack of Long-Term Maintenance
Full-arch restorations are not “maintenance-free.”
They require:
professional cleaning
screw and implant monitoring
bite adjustments
evaluation of wear
hygiene coaching
Without follow-up care, even well-designed restorations can fail prematurely.
Can Failed Full-Arch Cases Be Corrected?
In many cases, yes.
However, revision treatment is often more complex than initial treatment.
It may involve:
redesigning the prosthesis
replacing materials
correcting bite relationships
treating infections
repositioning implants
rebuilding bone
retraining hygiene techniques
Correcting a case requires understanding why it failed, not simply replacing what broke.
What Defines a “Fix-It” Office?
Offices experienced in revision and complication management typically:
✔ Plan prosthetically first
✔ Analyze failures instead of repeating them
✔ Customize each case
✔ Monitor patients long-term
✔ Educate patients honestly
✔ Expect complexity
Seeing difficult cases does not mean poor quality. It means the team understands real-world challenges — and how to prevent them.
Questions to Ask Before Choosing a Provider
Patients should ask:
• Who designs my teeth?
• Is my bite planned before surgery?
• How will speech be evaluated?
• What materials will be used and why?
• Who manages maintenance?
• What happens if something breaks?
• What is the plan if an implant fails?
The quality of the answers matters more than how fast the surgery can be done.
A Word About Cost
Lower-cost treatment often focuses on:
implant placement
standardized prosthetics
limited follow-up
Comprehensive care includes:
extensive planning
customized design
multiple prototypes
long-term maintenance
in-house management of complications
The true cost is not what is paid initially — it is what must be paid if treatment fails.
Our Philosophy
We believe full-arch treatment should be:
• designed before it is placed
• tested before it is finalized
• monitored for life
• customized for each patient
• managed by a coordinated team
• built to function, not just to look good
Some patients come to us for their first full-arch restoration.
Others come because something did not work elsewhere.
Both deserve careful planning and honest guidance.
The Bottom Line
Full-arch dental implants can be life-changing — but they are not simple.
When problems occur, they usually result from design, bite, or maintenance issues that develop over time.
The good news is:
many problems are preventable
many failures can be corrected
experienced teams can manage complex cases
If you are considering full-arch treatment — or struggling with an existing restoration — seek care from a team that treats this as a long-term rehabilitation, not just a surgical procedure.
Your smile is not a product.
It is a system.
And systems require thoughtful design.
All-on-4 Implants: Understanding Your Prosthesis Material Options
Choosing the right material for your All-on-4 implants is about more than looks. Learn how acrylic, composite, porcelain, and zirconia affect durability, hygiene, and long-term implant health.
All-on-4 Implants: Understanding Your Prosthesis Material Options
If you’re considering All-on-4 dental implants, you’ve probably heard your dentist mention different materials for your new teeth. The choice of material isn’t just about how your smile looks — it also affects your comfort, oral health, and how long your prosthesis will last. In this article, we’ll break down the main materials used for All-on-4 prostheses, explain their pros and cons, and help you understand what’s best for your mouth and lifestyle.
What is an All-on-4 Prosthesis?
Before we dive into materials, let’s quickly review what an All-on-4 prosthesis is.
All-on-4 is a treatment for people who are missing most or all of their teeth in one arch (upper or lower).
It uses four strategically placed dental implants to support a full arch of teeth.
The prosthesis can be made from different materials, each with its own strengths, longevity, and maintenance requirements.
Choosing the right material is important because it impacts how clean your teeth stay, how durable your prosthesis is, and how your gums and bone respond over time.
The Main Material Options
1. Acrylic Hybrid Prosthesis (PMMA)
What it is:
Acrylic is a type of resin, similar to the material used in dentures.
It’s often combined with a metal bar underneath for support.
Pros:
Lightweight and comfortable.
Easy to repair or adjust if something breaks.
Usually less expensive upfront.
Often used as a temporary or “conversion” prosthesis after implant surgery.
Cons:
Porous material: absorbs bacteria, odors, and stains over time.
High plaque retention: more likely to cause gum inflammation if cleaning isn’t perfect.
Wears down faster than other materials, especially for people who grind or clench their teeth.
Best for:
Temporary or transitional prosthesis.
Patients with excellent oral hygiene who want a lower-cost option.
2. Composite Hybrid Prosthesis
What it is:
Composite materials are a type of modern resin that’s reinforced with ceramic particles.
Often combined with a metal or titanium substructure.
Pros:
Less porous than acrylic, so it accumulates less plaque.
More durable and wear-resistant than acrylic.
Can be polished to a smooth finish, which is gentler on gums and opposing teeth.
Cons:
Still resin-based, so some plaque retention and staining can occur.
Repairs are easier than porcelain or zirconia, but not as simple as acrylic.
May need replacement sooner than zirconia.
Best for:
Mid-term prosthesis.
Patients who want a balance between cost, durability, and hygiene.
3. Porcelain on Titanium Framework
What it is:
Porcelain teeth are layered onto a strong titanium framework.
This is sometimes called a “metal-ceramic” prosthesis.
Pros:
Beautiful esthetics: porcelain can mimic natural tooth translucency and shading.
Very strong under normal bite forces.
Long clinical history — dentists have been using this approach for decades.
Cons:
Cement or veneer interfaces: the junction between porcelain and titanium can trap bacteria if not perfectly sealed.
Porcelain can chip over time, especially in patients who grind their teeth.
Harder to repair than acrylic or composite.
Best for:
Patients with high esthetic demands.
Those who want predictable long-term fit and passive implant support.
4. Monolithic Zirconia Prosthesis
What it is:
A prosthesis milled from a single block of zirconia, a very hard ceramic.
Can be full-arch zirconia or zirconia bonded over a titanium framework.
Pros:
Best biologic option: non-porous, highly polishable, and resistant to plaque buildup.
Extremely durable: rarely chips or fractures.
Ideal for bruxers: strong enough to withstand grinding or clenching.
Can look natural with proper shading and characterization.
Cons:
Very rigid — transmits biting forces directly to implants, so occlusion and implant placement must be precise.
Difficult to modify or repair chairside.
Higher cost than acrylic or composite.
Best for:
Long-term definitive prosthesis.
Patients with history of gum disease, high plaque risk, or heavy bite forces.
Anyone who wants the cleanest, most durable option.
5. Zirconia on Titanium Framework
What it is:
A hybrid approach: a zirconia shell is bonded over a titanium substructure.
Aims to combine zirconia’s hygiene benefits with titanium’s mechanical reliability.
Pros:
Smooth zirconia surface for optimal gum health.
Titanium bar absorbs stress and improves fit over long spans.
Easier to repair the framework if the zirconia shell chips.
Cons:
Cement or bonding layer can trap bacteria if not done perfectly.
Slightly more technique-sensitive than full monolithic zirconia.
Bulkier than monolithic zirconia, which may make cleaning slightly harder.
Best for:
Patients needing both high esthetics and long-span mechanical strength.
Bruxers with challenging bite forces.
Complex implant cases with angled or misaligned implants.
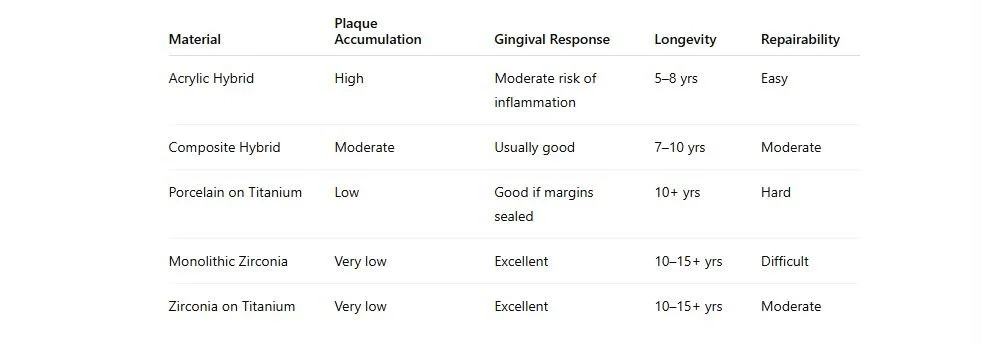
How Material Choice Affects Your Oral Health
The health of your gums and implants isn’t just about brushing and flossing — it’s also about what your teeth are made of:
Key takeaway: smooth, non-porous surfaces (zirconia, porcelain) are healthiest for your gums. Porous resins (acrylic, composite) require extra attention to prevent gum inflammation and plaque buildup.
Maintenance Considerations
Regardless of material, your prosthesis needs regular care:
Daily home care: water flosser, soft toothbrush under the prosthesis, low-abrasive toothpaste.
Professional cleanings: 3–4 times per year to remove any biofilm under the prosthesis.
Check-ups: regular evaluation of implants, gums, and bite forces.
Occlusion: especially important for bruxers — even the strongest prosthesis can fail if biting forces are not well-distributed.
Monolithic zirconia and zirconia-on-titanium generally require less frequent adjustments and tolerate grinding better than acrylic or porcelain.
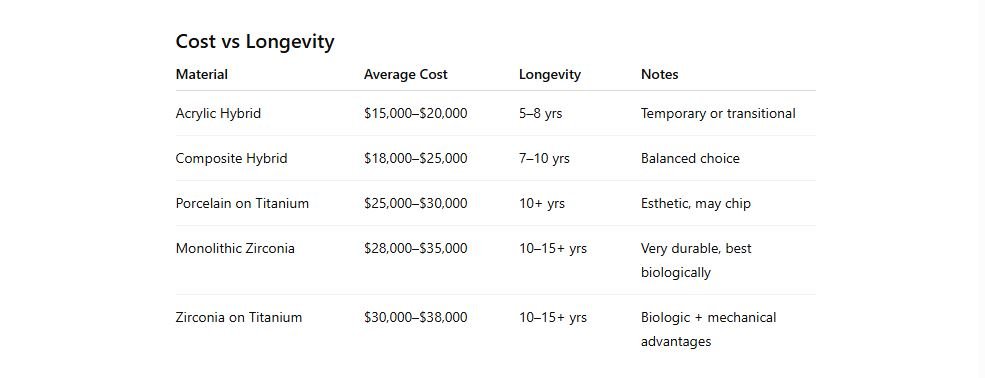
Investing in a higher-end prosthesis may save money long-term by reducing repairs, protecting implants, and minimizing gum inflammation.
How to Choose the Right Material
When deciding, your dentist will consider:
Oral hygiene habits
Bite forces / bruxism
Esthetic expectations
Bone quality and implant placement
Budget and long-term planning
Rule of thumb:
Acrylic → short-term / transitional
Composite → mid-term
Porcelain → esthetic-focused long-term
Monolithic zirconia → hygiene-focused long-term
Zirconia on titanium → high-strength, esthetic compromise
Final Thoughts
All-on-4 implants can transform your smile and your quality of life. Choosing the right prosthetic material ensures your new teeth last, stay healthy, and feel natural.
Monolithic zirconia and zirconia on titanium frameworks are generally best for long-term hygiene and durability.
Porcelain is unbeatable for esthetics but can chip under heavy forces.
Composite and acrylic hybrids are budget-friendly but require careful hygiene and more frequent replacement.
Ultimately, the “best” material depends on your mouth, lifestyle, and priorities. Discuss your options with your dentist, and consider not just appearance, but biologic health, durability, and maintenance.
Dental Veneers: What They Are, How They Work, and Whether They’re Right for You
Learn what dental veneers are, how they work, their benefits, lifespan, and whether they’re right for your smile. A complete patient guide to porcelain veneers.
If you’ve ever wished your teeth were whiter, straighter, or more even, you’re not alone. Dental veneers are one of the most popular cosmetic dentistry treatments because they can dramatically improve a smile while still looking natural.
But veneers are also one of the most misunderstood procedures. Many patients wonder:
Are veneers fake looking?
Do they ruin your teeth?
How long do they last?
Are they just for celebrities?
In this guide, we’ll explain what dental veneers are, who they’re for, how the process works, and what you should know before deciding if veneers are right for you.
What Are Dental Veneers?
Dental veneers are thin shells of porcelain or composite resin that are bonded to the front surface of your teeth. They are custom-made to match your natural teeth in color, shape, and size.
Veneers are designed to improve the appearance of teeth that are:
Chipped or worn
Discolored or stained
Uneven or misshapen
Gapped
Slightly crooked
Restored with large old fillings
Damaged from trauma
Unlike crowns, which cover the entire tooth, veneers only cover the front surface. This allows for a more conservative and cosmetic-focused approach.
What Problems Can Veneers Fix?
Veneers are extremely versatile. They are commonly used to treat:
1. Discoloration That Won’t Whiten
Some stains don’t respond to whitening, especially:
Tetracycline staining
Deep internal discoloration
Dark teeth from trauma or root canal treatment
Veneers can mask these stains and create a permanently brighter smile.
2. Chipped or Broken Teeth
Teeth that are chipped from wear, grinding, or trauma can often be restored with veneers rather than crowns.
3. Gaps Between Teeth
Small spaces between teeth can be closed with veneers without orthodontics in certain cases.
4. Uneven or Worn Teeth
Over time, teeth can become shorter or flatter due to grinding or acid wear. Veneers can restore length and symmetry.
5. Mild Crookedness
For patients who want fast cosmetic improvement and are not candidates for orthodontics, veneers can sometimes visually straighten teeth.
Types of Veneers
Porcelain Veneers
Porcelain veneers are the most durable and natural-looking option.
Benefits:
Highly stain resistant
Strong and long-lasting
Very natural translucency
Custom crafted by a dental lab
Porcelain veneers typically last 10–15 years or longer with good care.
2. Composite Veneers
Composite veneers are made from tooth-colored resin and placed directly on the teeth.
Benefits:
Less expensive than porcelain
Can often be done in one visit
Less tooth reduction required
They do not last as long as porcelain veneers and may stain over time.
The Veneer Process: Step by Step
One of the biggest fears patients have is not knowing what to expect. Here’s how the veneer process usually works:
Step 1: Consultation and Smile Planning
This is the most important step. Your dentist will:
Examine your teeth and bite
Take photos and digital scans
Discuss your goals
Evaluate gum health and jaw function
In many practices, digital smile design or mockups can show you what your new smile may look like before any work is done.
Step 2: Tooth Preparation
A small amount of enamel is removed from the front of the teeth to make room for the veneers. This ensures they don’t look bulky.
Local anesthesia is used, and the procedure is typically comfortable.
Step 3: Temporary Veneers
Temporary veneers are placed while your permanent veneers are being made. These allow you to:
Preview your smile
Test function and comfort
Give feedback on shape and size
Step 4: Final Veneer Placement
When the permanent veneers arrive:
They are tried in for fit and color
Adjustments are made
They are permanently bonded in place
This appointment usually takes 1–2 hours.
Do Veneers Look Natural?
When properly designed, veneers should not look fake. The most natural veneers:
Have slight translucency
Are shaped to match your face
Follow natural tooth proportions
Respect your bite and lip movement
Problems happen when veneers are:
Too thick
Too white
Poorly shaped
Placed without proper planning
A skilled cosmetic dentist will design veneers that look like healthy natural teeth — not “piano keys.”
Do Veneers Damage Your Teeth?
This is a common myth. Veneers do not ruin healthy teeth when properly planned and placed.
However, it is important to understand:
Veneers are not reversible
Enamel is permanently altered
Teeth will always need some form of coverage after veneers
That’s why proper case selection is critical. Veneers should only be placed when:
Teeth are structurally healthy
Gum health is stable
Bite forces are controlled
Long-term maintenance is understood
In the right hands, veneers can actually protect weakened or worn teeth.
How Long Do Veneers Last?
Porcelain veneers typically last 10–15 years, and sometimes longer.
Their lifespan depends on:
Oral hygiene
Grinding or clenching habits
Diet (hard foods, ice chewing)
Regular dental visits
Patients who grind their teeth may need a night guard to protect their veneers.
Are Veneers Painful?
Most patients report little to no pain during the veneer process.
Local anesthesia is used during tooth preparation
Temporary veneers protect the teeth
Sensitivity is usually mild and temporary
If sensitivity occurs, it typically resolves within days to weeks.
Who Is a Good Candidate for Veneers?
You may be a good candidate if:
Your teeth are healthy
Your gums are healthy
You want cosmetic improvement
You understand long-term maintenance
You don’t have uncontrolled grinding
You have realistic expectations
You may not be a candidate if:
You have advanced gum disease
You have untreated decay
You have severe bite problems
You grind heavily without protection
In those cases, other treatments may be recommended first.
Veneers vs. Crowns: What’s the Difference?
VeneersCrownsCover the front surfaceCover the entire toothMore conservativeMore tooth reductionPrimarily cosmeticCosmetic and structuralBest for healthy teethBest for damaged teeth
Your dentist will recommend the option that best protects your tooth long-term.
Veneers vs. Whitening
Teeth whitening can brighten natural teeth, but:
It cannot fix shape
It cannot fix chips
It cannot fix alignment
It cannot mask deep stains
Veneers can change:
Color
Shape
Size
Symmetry
Alignment appearance
For some patients, whitening is enough. For others, veneers provide a more complete transformation.
Caring for Veneers
Veneers are cared for like natural teeth:
Brush twice daily
Floss daily
Avoid biting hard objects
Wear a night guard, if recommended
See your dentist regularly
They cannot decay, but the underlying tooth can. Good hygiene is essential.
Common Myths About Veneers
Myth: Veneers look fake
Truth: Poorly done veneers look fake. Well-designed veneers look natural.
Myth: Veneers are only for celebrities
Truth: Veneers are common among everyday patients who want to improve their smile.
Myth: Veneers always require shaving teeth down to pegs
Truth: Modern veneers require minimal enamel reduction in many cases.
Myth: Veneers are purely cosmetic and unnecessary
Truth: Veneers can restore function and protect damaged teeth in addition to improving appearance.
Is Getting Veneers a Big Decision?
Yes — and it should be.
Veneers are a long-term investment in your smile and your oral health. A good veneer plan should consider:
Facial balance
Gum health
Bite stability
Longevity
Maintenance
Esthetics
This is not a one-size-fits-all procedure.
Final Thoughts: Are Veneers Worth It?
For the right patient, veneers can be life-changing. They can:
Improve confidence
Restore worn or damaged teeth
Create a balanced, healthy-looking smile
Provide long-lasting results
But they should never be rushed or poorly planned. The best results come from careful diagnosis, conservative preparation, and thoughtful design.
If you’re considering veneers, the most important step is a thorough consultation with a dentist who understands both esthetics and function.
Frequently Asked Questions About Veneers
How many veneers do I need?
It depends on your smile. Some patients need only two veneers, others need six to ten for symmetry.
Can veneers fall off?
Properly bonded veneers rarely fall off. Trauma or grinding can increase the risk.
Can I whiten veneers later?
No. Veneers do not whiten. Color must be chosen carefully before placement.
Are veneers covered by insurance?
Most veneers are considered cosmetic and not covered, though exceptions exist when restoring damaged teeth.
Ready to Take the Next Step?
A veneer consultation allows your dentist to evaluate your teeth, discuss your goals, and determine whether veneers are the right solution for your smile.
A great smile is not about perfection — it’s about balance, health, and confidence.
Why Do All-on-4 Cases Fail?
All-on-4 dental implants can fail if critical steps are missed. Learn the most common reasons All-on-4 cases fail — and how experienced implant teams prevent complications.
Understanding the Risks — and How They’re Prevented
All-on-4 dental implants have transformed the lives of millions of patients by offering a fixed, natural-looking alternative to dentures — often in just one day. When planned and executed correctly, All-on-4 is a predictable, long-lasting solution for patients with missing or failing teeth.
However, like any advanced medical or dental procedure, All-on-4 can fail under certain conditions.
If you’re researching All-on-4 implants, you may have come across conflicting information online — success stories on one side, warnings and horror stories on the other. The truth lies in understanding why failures occur and, more importantly, how experienced teams prevent them.
This article breaks down the most common reasons All-on-4 cases fail, what patients should watch for, and how proper planning dramatically reduces risk.
What Does “All-on-4 Failure” Actually Mean?
Before discussing causes, it’s important to define failure.
An All-on-4 case may be considered unsuccessful if:
One or more implants fail to integrate with bone
The prosthesis fractures or loosens repeatedly
Chronic pain, infection, or inflammation develops
The bite causes damage to implants or prosthetic teeth
The final result does not function or feel stable long-term
Failure doesn’t always mean total loss of the case — but it does mean additional procedures, delays, or compromises that could have been avoided.
1. Inadequate Diagnosis and Treatment Planning
This is the most common root cause of All-on-4 failure.
All-on-4 is not a “one-size-fits-all” procedure. Success depends on:
Bone volume and density
Bite forces
Jaw position
Medical history
Esthetic and functional expectations
Where Things Go Wrong
No 3D CBCT imaging
Limited evaluation of bone quality
Failure to assess parafunction (clenching/grinding)
Rushed treatment plans driven by speed or cost
Without comprehensive planning, implants may be placed in compromised bone or at angles that overload them over time.
How Failures Are Prevented
Full 3D CBCT analysis
Digital implant planning
Occlusal and bite assessment
Risk stratification before surgery
2. Poor Implant Placement or Angulation
All-on-4 relies on strategic implant angulation to maximize existing bone and avoid grafting. When done correctly, this increases stability. When done incorrectly, it increases risk.
Common Placement Errors
Implants placed too shallow or too deep
Improper angulation causing uneven force distribution
Failure to engage dense cortical bone
Overheating bone during placement
Even small errors can lead to micromovement, preventing implants from properly integrating.
Prevention
Guided or digitally planned surgery
Proper torque values and insertion protocols
Experienced surgical judgment (not just software reliance)
3. Overloading the Implants Too Soon
“All teeth in one day” is appealing — but immediate loading must be done carefully.
Temporary teeth placed on implants too early or designed incorrectly can overload healing implants.
Risk Factors
Excessive bite forces
Hard or inflexible temporary materials
Patients not following soft-food protocols
Undiagnosed clenching or grinding
How Experienced Teams Prevent This
Designing provisional prostheses with protective occlusion
Limiting bite forces during healing
Strict post-op dietary instructions
Night guards when indicated
4. Poor Prosthetic Design
All-on-4 success depends just as much on prosthetic engineering as surgical skill.
Common Prosthetic Failures
Fractured acrylic or teeth
Loosening of screws
Excessive cantilever length
Poor bite alignment
If the prosthesis does not distribute forces evenly, implants can fail even if surgery was technically perfect.
Prevention
Collaboration between surgeon and restorative team
Proper framework design
Balanced occlusion
Materials selected based on patient force levels
5. Untreated Infection or Peri-Implantitis
Infection around implants can compromise bone support and stability.
Causes
Residual infection from failing teeth
Poor oral hygiene access
Smoking
Poorly contoured prostheses that trap plaque
Prevention
Thorough debridement at surgery
Proper antibiotic protocols when indicated
Prosthetic designs that allow cleanability
Long-term maintenance programs
6. Patient-Related Risk Factors
Some failures are related to patient health or habits — not the procedure itself.
Higher-Risk Factors
Heavy smoking or vaping
Uncontrolled diabetes
Severe clenching or grinding
Poor compliance with instructions
Missed follow-up appointments
These don’t automatically disqualify patients — but they must be identified and managed.
Risk Reduction Strategies
Medical coordination when necessary
Smoking cessation counseling
Occlusal guards
Clear expectations and education
7. Lack of Experience With Complex Cases
All-on-4 is not just “placing implants.”
It requires:
Advanced surgical judgment
Prosthetic planning expertise
Experience managing complications
A coordinated team approach
Why Experience Matters
Complications aren’t always avoidable — but experienced teams know how to prevent small issues from becoming failures.
How Often Do All-on-4 Implants Fail?
When performed by experienced teams:
Implant survival rates are typically 95–98% or higher
Most complications are manageable and prosthetic, not surgical
Failures are far more likely when shortcuts are taken in planning, execution, or follow-up.
How to Protect Yourself as a Patient
If you’re considering All-on-4, ask these questions:
Will you use a CBCT scan for planning?
Who designs the prosthesis — and how?
What materials are used for temporary and final teeth?
How do you manage bite forces?
What happens if a complication occurs?
The answers matter more than price.
Final Thoughts: All-on-4 Failures Are Largely Preventable
All-on-4 dental implants are one of the most successful treatments in modern dentistry — when done correctly.
Most failures stem from:
Inadequate planning
Poor execution
Lack of experience
Misaligned expectations
Choosing the right team dramatically reduces risk and increases long-term success.
If you’re exploring All-on-4, education is your greatest protection.
All-on-4 vs. Traditional Dental Implants: Which Is Best for You?
Compare All-on-4 dental implants vs traditional implants. Learn about cost, recovery, longevity, and which option is best for full-arch tooth replacement in NH.
Understanding Your Implant Options
If you’re researching dental implants, you’ve likely come across two common options: All-on-4 dental implants and traditional dental implants. Both can restore missing teeth and improve your quality of life — but they are designed for very different needs.
Patients often ask:
Which option lasts longer?
Which one costs more?
Which one is less invasive?
Which is better if I’m missing most or all of my teeth?
At All-on-4 NH, we help patients from Hanover, Manchester, Dover, and across New Hampshire navigate these decisions every day. This guide explains the differences clearly, so you can make an informed choice that fits your health, goals, and lifestyle.
What Are Traditional Dental Implants?
Traditional dental implants are designed to replace one missing tooth at a time. Each implant consists of a titanium post placed into the jawbone, which acts as an artificial tooth root. Once the implant integrates with the bone, a crown is placed on top.
This approach works extremely well when:
One or a few teeth are missing
The surrounding teeth are healthy
Adequate bone is present at each implant site
However, when many teeth are missing, traditional implants can become complex, time-consuming, and expensive.
What Is the All-on-4 Implant Approach?
All-on-4 is a full-arch implant solution that replaces an entire upper or lower set of teeth using only four strategically placed implants. Two implants are placed vertically in the front of the jaw, and two are angled in the back to maximize bone support.
This technique allows:
Fewer implants to support more teeth
Reduced need for bone grafting
Faster overall treatment time
Immediate placement of temporary teeth in many cases
All-on-4 is often referred to as “teeth in a day” because patients can leave surgery with a functional smile.
Major Differences Between All-on-4 and Traditional Implants
1. Number of Implants Required
Traditional implants typically require one implant per missing tooth or, in some cases, 6–10 implants per arch to support a full bridge. This increases surgical time, healing periods, and overall cost.
All-on-4 uses just four implants to support an entire arch of teeth, making it far more efficient for patients missing most or all of their teeth.
2. Treatment Time and Healing
With traditional implants, treatment often takes 9–18 months when replacing multiple teeth. Each implant may require:
Bone grafting
Healing time after placement
Additional procedures before final crowns are placed
All-on-4 significantly shortens this timeline. Many patients receive:
Implant placement and temporary teeth on the same day
Final teeth within 3–6 months after healing
For patients eager to restore function and confidence quickly, this difference is substantial.
3. Bone Grafting Requirements
Traditional implants require sufficient bone at each implant site. If bone loss is present — which is common in long-term denture wearers — bone grafting is often necessary.
All-on-4 implants are angled strategically to use existing bone, often eliminating the need for bone grafting entirely. This makes All-on-4 an excellent option for patients who were previously told they were “not candidates” for implants.
4. Cost Considerations
Traditional implants can be cost-effective for single-tooth replacement, but costs increase rapidly when multiple implants are needed. Replacing a full arch with traditional implants often becomes prohibitively expensive due to:
Multiple surgeries
Bone grafting
Individual crowns or bridges
All-on-4 is generally more cost-effective for full-arch replacement because it uses fewer implants, fewer surgeries, and a streamlined prosthetic process.
While All-on-4 still represents a significant investment, many patients find it offers better long-term value compared to dentures or extensive traditional implant work.
5. Stability and Daily Function
Traditional implants offer excellent stability for individual teeth. However, when many implants are placed, patients may experience prolonged periods without teeth during healing.
All-on-4 patients typically enjoy:
Immediate stability with temporary teeth
No slipping or adhesives like dentures
Improved ability to chew and speak confidently
This immediate functional improvement is one of the most life-changing aspects of All-on-4 treatment.
6. Maintenance and Longevity
Both All-on-4 and traditional implants are designed to be long-lasting solutions.
Traditional implants, when properly cared for, can last decades. Individual crowns may need replacement over time due to wear.
All-on-4 implants also have excellent longevity, often lasting 20+ years with good oral hygiene and regular dental visits. The prosthetic teeth may need maintenance or replacement over time, similar to any dental restoration.
Which Option Is Better for Full Tooth Loss?
If you are missing most or all of your teeth, All-on-4 is usually the preferred option because it:
Minimizes surgery
Reduces treatment time
Avoids removable dentures
Restores function and aesthetics quickly
Traditional implants are better suited for:
Replacing one or two missing teeth
Patients with strong bone at specific sites
Situations where a full-arch solution is not needed
Common Patient Questions
Is All-on-4 less durable because it uses fewer implants?
No. The implants are strategically placed to distribute biting forces efficiently, providing excellent long-term stability.
Does All-on-4 look natural?
Yes. The prosthetic teeth are custom-designed to match your facial features, smile, and natural tooth shape.
Can I start with dentures and switch to All-on-4 later?
Yes, many patients transition from dentures to All-on-4 when they’re ready for a more permanent solution.
Which option hurts less?
Both procedures are performed with sedation for comfort. All-on-4 often involves less overall surgical trauma due to fewer implants.
Financing and Accessibility
Both traditional implants and All-on-4 represent an investment in your health and quality of life. At All-on-4 NH, we offer:
Flexible monthly financing options
Third-party payment plans
Transparent cost discussions during your consultation
For many patients, All-on-4 provides a more predictable and affordable path to full-mouth restoration.
Making the Right Choice for You
Choosing between All-on-4 and traditional implants depends on:
How many teeth you’re missing
Your bone health
Your desired timeline
Your budget and long-term goals
That’s why a personalized consultation is essential. During your visit, we’ll evaluate your oral health, discuss both options, and help you choose the solution that best fits your needs.
Take the Next Step
If you’re considering dental implants in Hanover, Manchester, or anywhere in New Hampshire, we invite you to take the next step:
Take our 60-second eligibility quiz
Schedule a personalized implant consultation
Learn which option is best for your smile
👉 Visit All-on-4NH.com to get started today.
Common Misconceptions About All-on-4 Dental Implants (And the Truth Behind Them)
Confused about All-on-4 dental implants? Learn the most common myths and misconceptions — and the real facts — so you can make a confident, informed decision.
Why So Many Patients Feel Confused About All-on-4
If you’ve researched All-on-4 dental implants online, you’ve probably encountered conflicting information. Some sources make it sound too good to be true. Others make it seem risky, painful, or experimental.
This confusion leads many patients to delay treatment — even when All-on-4 could dramatically improve their quality of life.
At The Dental Center, we hear the same concerns from patients across Hanover, Manchester, Dover, and throughout New Hampshire. This article addresses the most common misconceptions about All-on-4 dental implants and explains the truth behind each one.
Misconception #1: “All-on-4 Is Too New or Experimental”
This is one of the most common fears — and one of the most inaccurate.
The truth: All-on-4 has been used worldwide for over 20 years and is supported by extensive clinical research. The technique was developed to maximize stability while minimizing the need for bone grafting.
Today, All-on-4 is a well-established, predictable treatment when performed by an experienced implant team using proper planning and materials.
Misconception #2: “You Only Get Four Implants — That Can’t Be Strong Enough”
The number “four” understandably makes some patients nervous.
The truth: All-on-4 uses strategic implant placement, not random placement. Two implants are placed vertically in the front, where bone density is strongest. Two implants are placed at an angle in the back to maximize contact with available bone.
This design:
Distributes chewing forces efficiently
Provides excellent long-term stability
Often avoids the need for bone grafting
In many cases, All-on-4 is just as strong — or stronger — than traditional approaches using more implants.
Misconception #3: “I’ll Be Without Teeth While Everything Heals”
Many patients fear months of being toothless.
The truth: Most All-on-4 patients leave surgery the same day with a fixed, temporary set of teeth. These teeth are attached to the implants and are not removable.
While they are designed to protect the implants during healing, they allow you to:
Smile confidently
Speak clearly
Eat soft foods
You are never expected to go without teeth during the healing phase.
Misconception #4: “All-on-4 Is Only for Older Patients”
Some people assume implants are only for seniors.
The truth: All-on-4 is used for adults of many ages. Patients seek this treatment due to:
Failing crowns and bridges
Advanced gum disease
Severe tooth wear
Genetic dental issues
Long-term denture frustration
What matters is oral health, bone structure, and overall medical stability, not age alone.
Misconception #5: “The Surgery Is Extremely Painful”
Fear of pain keeps many people from scheduling a consultation.
The truth: All-on-4 surgery is typically performed with:
IV sedation
Oral sedation
Local anesthesia
Most patients report less discomfort than expected, often comparing it to or less than traditional tooth extractions.
Post-operative soreness is normal but usually manageable with medication and proper aftercare. Many patients return to light activities within a few days.
Misconception #6: “Dental Implants Fail All the Time”
Online horror stories can be alarming.
The truth: Dental implants — including All-on-4 — have a very high long-term success rate when placed properly and maintained well.
Factors that improve success include:
Proper diagnosis and planning
Skilled surgical placement
Good oral hygiene
Regular follow-up care
Failures are uncommon and often related to unmanaged health conditions or smoking.
Misconception #7: “All-on-4 Looks Fake or Bulky”
Some patients worry their smile will look unnatural.
The truth: Modern implant prosthetics are designed with:
Natural tooth proportions
Customized shape and color
Proper lip and facial support
Your final teeth are custom-designed specifically for your face, not generic dentures. Most people notice how natural your smile looks — not that you’ve had dental work.
Misconception #8: “All-on-4 Is Only About Appearance”
While the cosmetic transformation is dramatic, All-on-4 is about much more than looks.
The truth: All-on-4 restores:
Proper chewing function
Jawbone stimulation
Clear speech
Facial structure support
It also eliminates the daily frustration of loose dentures, adhesives, and dietary limitations.
Misconception #9: “It Takes Years to Finish the Process”
Some patients assume implants are a multi-year ordeal.
The truth: The typical All-on-4 timeline is 3–6 months from surgery to final teeth. Many patients feel functional and confident much sooner because they receive temporary teeth immediately. Compared to traditional implant approaches, All-on-4 is often faster and more streamlined.
Misconception #10: “All-on-4 Is Never Affordable”
Cost is a real concern — but assumptions often prevent patients from exploring options.
The truth: All-on-4 can be more cost-effective long-term than:
Replacing failing crowns repeatedly
Ongoing denture adjustments
Bone grafting-heavy implant plans
At The Dental Center, we focus on:
Transparent pricing
Financing options with monthly payments
Helping patients plan treatment realistically
Many patients are surprised to learn it’s more attainable than they expected.
Why These Misconceptions Persist
Much of the confusion comes from:
Outdated online information
General dental websites that don’t specialize in implants
Lack of personalized evaluation
That’s why a comprehensive consultation is essential. Your situation is unique, and generalized advice can be misleading.
The Importance of an Experienced Implant Team
All-on-4 outcomes depend heavily on:
Surgical experience
Prosthetic design
Long-term maintenance planning
Choosing a team that performs All-on-4 regularly — not occasionally — significantly reduces risks and improves results.
Take the Next Step with Confidence
If you’ve been hesitant because of something you’ve heard or read, you’re not alone. The best way to move forward is with accurate information and a personalized plan.
At The Dental Center, we serve patients from Hanover, Manchester, Dover, and across New Hampshire, providing clarity, transparency, and expert care.
👉 Take our 60-second eligibility quiz
👉 Schedule a consultation
👉 Get answers tailored to you
Visit All-on-4NH.com to take the next step.
Do I Need a Crown or a Filling? How to Know Which Treatment Is Right for Your Tooth
Learn whether you need a dental crown or filling based on decay size, cracks, and tooth strength. Understand treatment options and protect your long-term oral health.
When you’re told that you need dental treatment, one of the most common questions is: “Do I really need a crown, or will a filling be enough?”
It’s a fair question. Both fillings and crowns restore teeth, but they do so in very different ways. The right choice depends on the amount of damage, location of the tooth, existing restorations, risk of future fracture, and long-term prognosis. Understanding the difference helps you make a confident decision about your oral health, your investment, and your long-term comfort.
In this guide, we’ll break down how dentists determine whether a filling or a crown is appropriate, what each procedure involves, and how to know which option gives your tooth the best chance of long-lasting success.
What a Filling Does: Repairing Small to Moderate Decay
A filling—whether composite (tooth-colored) or amalgam—is designed to replace tooth structure lost to decay or small fractures.
Fillings are appropriate when:
The cavity is small to moderate in size
The tooth structure around the decay is strong
There are no large cracks
The tooth hasn’t already been heavily restored
The decay hasn’t spread under an existing restoration
How Fillings Work
The dentist removes the decayed portion of the tooth and replaces that missing portion with a durable restorative material. Composite resin bonds directly to the tooth, which helps maintain strength and prevent leakage.
Advantages of Fillings
Minimally invasive
Preserves more natural tooth structure
Often completed in one visit
Lower cost compared to a crown
Great longevity when conditions are right
Limitations of Fillings
Filling materials rely on remaining strong enamel for stability. When too much structure is gone, or the tooth is cracked, a filling simply can’t reinforce the tooth enough to prevent future breakage.
This is often where patients feel confused—because a filling is “smaller” treatment, but it isn’t always the safer option.
What a Crown Does: Protecting a Weakened Tooth
A crown covers the entire visible surface of the tooth like a strong, protective shell.
Crowns are recommended when:
The tooth has large decay or a large existing filling
There are visible cracks (like cracked tooth syndrome)
The enamel is weakened or missing
A portion of the tooth has fractured
The tooth has undergone root canal therapy
You need long-term reinforcement to prevent breaking
How Crowns Work
A crown is custom-designed to fit over the tooth, restoring its shape, function, and strength. Modern crowns—such as zirconia or e.max—are extremely strong and lifelike.
Advantages of Crowns
Reinforces the entire tooth
Prevents fractures and catastrophic tooth loss
Excellent long-term durability
Restores chewing efficiency and comfort
Ideal for teeth with cracks or after root canal
Limitations of Crowns
More of the tooth must be shaped compared to a filling
Higher cost
Usually requires two visits (unless your office offers same-day crowns)
Still, for many teeth, a crown provides far better longevity and reduces the risk of an emergency break that might require more extensive treatment later.
How Dentists Decide: Key Factors That Determine the Best Option
Patients sometimes believe dentists “just pick one,” but the decision is based on specific structural, biological, and mechanical factors. Here are the main considerations your provider is evaluating:
1. Size of the Cavity or Filling
The larger the area of decay, the more likely the tooth will benefit from a crown.
Small decay → Filling
Moderate decay → Gray area; may depend on tooth location
Large decay → Crown (filling would be unstable)
A large filling acts like a plug instead of reinforcement, increasing the risk of the tooth breaking later.
2. Presence of Cracks
Cracks change everything. Even if the cavity is small, a crack in the tooth can spread under pressure from chewing. A crown helps hold the tooth together, preventing it from splitting. Fillings cannot stop cracks from propagating.
3. Location of the Tooth
Back teeth (molars and premolars) take 80% of chewing force. They’re more prone to breaking when compromised. Front teeth usually tolerate fillings better because they experience lighter forces.
4. Structural Integrity After Decay Removal
Sometimes dentists can’t determine crown vs. filling until the decay is cleaned out. What remains must be thick, solid, and continuous. If removing decay leaves thin walls or unsupported cusps, a crown becomes the safer option.
5. Existing Restorations
A tooth can only hold so many fillings before it becomes structurally weak.
Teeth with:
Large fillings
Multiple previous fillings
Recurrent decay under old restorations
…usually require a crown for predictable long-term success.
6. Root Canal Treatment
Any tooth that has undergone a root canal becomes more brittle. Crowning these teeth significantly reduces the risk of fractures—sometimes catastrophic fractures that make the tooth non-restorable.
What Happens If You Choose a Filling When a Crown Was Needed?
This is the scenario dentists try hardest to avoid.
A tooth that should have been crowned but instead receives a filling is at risk for:
Cracking
Breaking during chewing
Needing a root canal
Losing more tooth structure
Needing emergency care later
Becoming non-restorable
Patients often say: “Why didn’t the filling fix it?” Because the filling cannot strengthen the tooth—it only replaces missing structure. If the tooth is weak, a filling is simply not enough.
What Happens If You Choose a Crown When a Filling Would Have Worked?
In this case, you may simply be overtreating. However, a crown will still protect the tooth and provide durability, even if a filling would have been adequate. It’s less risky than the reverse situation.
Good dentists will always explain the why behind their recommendation and use intraoral photos or digital scans so you can see the condition of the tooth yourself.
How to Feel Confident in Your Treatment Decision
Here are the signs your dentist is giving you a thoughtful, evidence-based recommendation:
🔹 They show you photos of the tooth
🔹 They explain the extent of damage
🔹 They discuss long-term expectations
🔹 They outline risks of both options
🔹 They respond openly to questions
🔹 They prioritize preserving natural tooth structure when appropriate
A transparent, visual explanation builds trust and helps you understand exactly why a crown or filling is recommended.
Bottom Line
Fillings and crowns are both excellent treatments—but they serve very different purposes.
Fillings are best for small to moderate decay and small fractures.
Crowns are best for large decay, cracks, weakened enamel, or after root canal therapy.
Choosing the right treatment protects your long-term dental health, prevents emergencies, and ensures you can chew comfortably and confidently for years.
If you’re unsure which option is right for you, ask to see images of your tooth and discuss long-term pros and cons. Your smile—and your investment—are worth making the most informed choice.
The All-on-4 Revolution: A New Smile in One Day
Imagine walking into the dental office with missing or failing teeth — and leaving the same day with a brand-new, fixed, natural-looking smile. That’s the promise of All-on-4 dental implants, a revolutionary treatment designed especially for patients who want a permanent solution without the wait, discomfort, or hassle of traditional dentures.
Using just four strategically placed implants, All-on-4 secures a full arch of new teeth in a single appointment — restoring your ability to eat, speak, and smile with total confidence. It’s fast, predictable, and life-changing.
At The Dental Center Collective, our team specializes in this transformative treatment, guiding patients through every step of the journey with comfort and care. If you’ve been told you’re “not a candidate” for implants or are tired of dentures, All-on-4 could be your key to freedom — and your best smile yet.
If you’ve been told you need full dentures, or if you’re tired of your current set, there’s a modern alternative that can change your life — All-on-4 dental implants.
This revolutionary procedure gives you a fixed, beautiful set of teeth in a single day — without months of waiting or painful bone grafting.
What Is All-on-4?
The All-on-4 treatment uses just four strategically placed dental implants to support a full arch of new teeth. The implants are angled to maximize existing bone, which means even patients with bone loss can often qualify.
In most cases, patients leave the same day with a full, functional smile.
How It Differs from Traditional Implants
Traditional implant cases may require one implant per missing tooth, bone grafting, and months of healing. All-on-4 simplifies that process — fewer implants, no grafting, and immediate results.
Benefits Patients Love
Instant results: Walk out with a new smile the same day.
Stable and strong: No slipping, clicking, or adhesives.
Natural look and feel: Designed to match your facial structure.
Preserves bone: Stimulates bone and prevents further loss.
Easier care: Just brush and floss like normal teeth.
Life After All-on-4
Patients often describe dramatic improvements:
Eating comfortably for the first time in years
Speaking clearly and smiling naturally
Renewed confidence in social and professional settings
One of our patients said, “It’s like I got my twenties back — not just my smile, but my energy.”
The Procedure: What to Expect
Consultation & 3D Scan: We evaluate bone density and create a digital plan.
Treatment Day: Damaged teeth are removed, implants placed, and temporary teeth secured — all in one visit.
Healing Phase: Over the next few months, implants fuse with bone.
Final Smile: Custom, permanent teeth are attached for a beautiful, lasting result.
Why Choose a Specialist Team
Experience matters. At The Dental Center Collective, our team of surgical and restorative specialists works together under one roof. You’ll enjoy seamless care, sedation options for comfort, and a smile that’s built to last.
The Confidence You Deserve
All-on-4 can restore not just your teeth — but your sense of freedom. You’ll smile bigger, laugh louder, and eat what you love again.
Your best years are still ahead. Let’s make sure your smile shows it.
Dental Implants vs. Dentures: The Real Cost of Confidence
When it comes to replacing missing teeth, many patients wonder whether dentures or dental implants are the right choice. While dentures may seem more affordable at first, they often come with hidden costs — slipping, discomfort, adhesives, and frequent replacements. Dental implants, on the other hand, provide a secure, natural-looking solution that can last decades while protecting your bone and facial structure.
This isn’t just about restoring your teeth — it’s about restoring your confidence, your diet, and your ability to live life without worry. If you’re ready to eat what you love again, smile freely, and enjoy the security of teeth that feel like your own, The Dental Center Collective can help you understand the difference implants can make.
A confident smile is priceless — and it’s never too late to invest in yours.
If you’ve lost one or more teeth, you’ve probably wondered whether dentures or dental implants are the better choice. At first glance, dentures seem more affordable — but when you consider comfort, long-term cost, and quality of life, implants often come out ahead.
Here’s a breakdown to help you make an informed, confident decision.
The Hidden Costs of Traditional Dentures
While dentures cost less initially, they often come with ongoing expenses:
Frequent relines or replacements due to bone loss
Adhesive products
Cleaning solutions and special maintenance
Possible dietary restrictions (softer foods, limited chewing ability)
Over 10–15 years, the cost of maintaining dentures often surpasses that of implants.
The Problem with Bone Loss
When teeth are missing, the jawbone begins to deteriorate. This causes dentures to loosen over time, making it harder to talk or eat comfortably. Dental implants, however, preserve the bone by mimicking a natural tooth root — keeping your face structure intact and your bite strong.
Comfort and Confidence in Daily Life
Imagine laughing with friends, eating in public, or giving a presentation without worrying that your dentures might slip. Implant-supported teeth are securely anchored, so you can live life without fear or discomfort.
Many patients say they feel like they have their natural teeth again — a freedom no removable denture can match.
Long-Term Investment in Health
Because implants stimulate the bone, they help prevent the sunken facial appearance often associated with aging. That means fewer wrinkles around the mouth and better support for lips and cheeks.
In addition, being able to chew a full range of foods contributes to better nutrition, digestion, and overall wellness.
Cost Comparison at a Glance
When comparing dentures and dental implants, there are several key differences to consider. Dentures typically have a lower initial cost, but over time, expenses add up due to frequent relines, replacements, adhesives, and specialized cleaning products. They can slip or irritate gums, don’t preserve bone, and usually need to be replaced every 5–10 years. In contrast, dental implants have a higher upfront cost, but they offer long-term value: they feel and function like natural teeth, preserve jawbone, and generally last 20 years or more with normal brushing and flossing. Implants also eliminate the need for adhesives or special maintenance and provide stability for everyday activities like eating, speaking, and smiling. For many patients over 55, the increased comfort, confidence, and longevity of implants make them a worthwhile investment compared with traditional dentures.
Who’s a Good Candidate for Implants?
Most adults in good general health can get implants, even those with some bone loss thanks to modern techniques like All-on-4.
If you’ve worn dentures for years, you may still be eligible for implants. A 3D scan can determine your options in minutes.
The Bottom Line
While dentures remain a valid option for some, dental implants offer unmatched comfort, confidence, and long-term value. They’re not just an investment in your smile — they’re an investment in how you live every day.
Why Your Smile Changes After 55 — And What You Can Do About It
As we age, subtle changes in our smile can start to affect how we look, eat, and feel. Teeth wear down, gums recede, and bone loss can alter the shape of your face. But these changes aren’t something you have to accept as “just part of getting older.” Modern dentistry offers powerful solutions that restore not only your smile but your confidence and comfort, too.
Whether it’s strengthening worn teeth, addressing gum health, or replacing missing teeth with long-lasting dental implants, there are ways to turn back the clock on your oral health. At The Dental Center Collective, we specialize in helping adults 55 and older reclaim the strong, beautiful smiles they deserve — comfortably and confidently.
Because your best years should come with your best smile.
By the time we reach our fifties and sixties, most of us notice subtle (or not-so-subtle) changes in our smile. Teeth may shift, gums recede, and the once-bright smile we had in our thirties might start to fade. These changes are a natural part of aging—but that doesn’t mean you have to live with them.
Understanding why your smile changes with age is the first step to keeping it healthy, confident, and functional for decades to come.
The Natural Aging Process of the Mouth
Just like skin and joints, the mouth undergoes changes over time. Some of the most common include:
Tooth wear: Years of chewing, grinding, and acid exposure gradually wear enamel.
Gum recession: Gums naturally thin and pull away from teeth, making them look longer and more sensitive.
Bone loss: After age 50, bone density begins to decline, including the jawbone that supports your teeth.
Dry mouth: Medications and hormonal changes reduce saliva, which protects against decay.
These small shifts can lead to loose teeth, bite changes, or dentures that no longer fit properly.
How Missing Teeth Accelerate Aging
When a tooth is lost, the bone underneath it begins to dissolve. Over time, this can cause the face to appear sunken or “collapsed.” Many patients describe looking older or tired, even if they feel young and vibrant inside.
Dental implants help stop this process by replacing the root of the tooth and preserving bone structure. This is one of the main reasons more patients over 55 are choosing implant-based solutions instead of removable dentures.
Restoring Function — Not Just Appearance
Today’s dental solutions go far beyond cosmetics. The goal is full oral rehabilitation — restoring the ability to chew, speak, and smile comfortably.
Dental implants: Permanent replacements that look and function like natural teeth.
Implant-supported dentures or bridges: Secure and stable, no slipping or adhesive.
All-on-4 full-arch treatment: A complete set of new teeth anchored by just four implants — ideal for patients with significant tooth loss.
Many patients describe feeling like they “got their life back” after treatment — enjoying steaks, apples, and laughter again without hesitation.
The Emotional Impact of a Healthy Smile
Confidence doesn’t retire at 55. In fact, this stage of life is often filled with new beginnings — travel, grandkids, dating again, or professional reinvention. A healthy, confident smile can profoundly affect how people see you and how you see yourself.
Numerous studies show that smiling can reduce stress hormones, lower blood pressure, and boost mood — all of which contribute to better overall health.
Taking the First Step
If it’s been a few years since your last dental checkup, you’re not alone. Many adults avoid the dentist after negative past experiences. The good news: modern dentistry is gentler, faster, and more comfortable than ever before.
At The Dental Center Collective, we specialize in care for adults and seniors — with advanced technology that minimizes discomfort and maximizes results.
Your next chapter deserves a confident smile.
The Hidden Costs of Cheap Dental Implants — What Patients Need to Know
Many patients are price-shopping and searching for “affordable dental implants.” This lets you educate and differentiate your premium care model. We will discuss the true cost of failed or low-quality treatment versus long-term investment in precision and expertise
When “Cheap” Dental Implants End Up Costing More
It’s natural for patients to compare prices when researching full-mouth dental implants. After all, it’s a major investment in your health, confidence, and quality of life.
But there’s a growing concern across New England — more patients are arriving at specialty clinics like The Dental Center Collective with complications from low-cost or overseas implant procedures.
At first glance, a cheaper option may sound appealing. Yet what’s often left out of the conversation is the true cost — in comfort, longevity, and future re-treatment.
What Makes Some Implants “Cheap”?
Low-cost implant centers often reduce prices by cutting corners in ways that most patients can’t see, such as:
Using generic or off-brand implants that aren’t backed by long-term data or global support.
Skipping digital planning tools like 3D imaging or photogrammetry, which are key to precision.
Rushing surgical timelines or skipping proper healing periods.
Relying on acrylic teeth instead of long-lasting zirconia or hybrid prosthetics.
High-volume, low-touch care models where every patient receives the same template plan.
Each of these shortcuts can compromise the accuracy, comfort, and longevity of your final result.
The Real-World Cost of Implant Failure
When cheap implants fail — and they often do — the consequences can be serious:
Bone loss or infection that makes future treatment more difficult.
Pain, swelling, or loosening of the prosthesis.
The need to remove and replace implants, often requiring bone grafting.
Emotional and financial strain from redoing treatment that was meant to last.
Rehabilitation after failed implant work can cost 2–3x more than doing it right the first time.
Why Quality Treatment Pays Off
At The Dental Center Collective, we focus on the long-term value of your smile — not the lowest price tag.
Our All-on-4 patients benefit from:
✅ Digital implant planning for maximum precision and minimal discomfort.
✅ Photogrammetry and guided surgery for exact prosthetic fit and bite alignment.
✅ Premium materials like titanium implants and zirconia restorations for strength and beauty.
✅ Collaborative prosthodontic and surgical expertise, ensuring seamless function and aesthetics.
Investing in quality care means your smile is designed to last decades — not years.
A New England Perspective
Patients across New Hampshire, Massachusetts, and Maine are increasingly seeking second opinions after realizing that “discount implant deals” don’t always tell the full story.
Our goal is to help patients make informed decisions, grounded in transparency, precision, and trust.
If you’ve been quoted a surprisingly low price elsewhere, it’s worth asking:
What brand of implants will be used?
Is the surgery guided digitally?
Who is restoring the final prosthesis?
What happens if something goes wrong?
Is a multi-year warranty included?
Protect Your Health — and Your Investment
Dental implants are a life-changing procedure — not a commodity.
Choosing an experienced, technology-driven team ensures your treatment is safe, durable, and truly customized for you.
At The Dental Center Collective, we help patients throughout New England regain confidence with full-arch implant solutions that are engineered for long-term success.
📍 Serving New Hampshire, Massachusetts, and surrounding regions.
📞 Schedule a consultation today to compare your options with clarity and confidence.
How Long Do All-on-4 Dental Implants Last?
Longevity and durability are top concerns for patients considering such a major investment. Discover how long All-on-4 dental implants can last, what affects their lifespan, and how New England patients can ensure lasting results with expert care.
A Lifetime Smile, Not a Temporary Fix
When patients in New England start researching full-mouth dental implants, one of the first questions they ask is: “How long will my All-on-4 implants last?”
The short answer: with proper planning, high-quality materials, and good oral hygiene, All-on-4 dental implants can last 20+ years — often a lifetime. But as with most major investments, longevity depends on how and where your treatment is done.
Why All-on-4 Implants Last So Long
All-on-4 dental implants are designed to replace an entire arch of missing teeth using just four to six implants. Unlike dentures, they are anchored securely in the jawbone, helping to prevent bone loss and maintain facial structure.
Here’s what gives them their durability:
Titanium Integration: The implants fuse directly with your jawbone (osseointegration), forming a permanent bond.
Precision Planning: When the surgery is guided digitally — using 3D imaging or photogrammetry — implant placement is more accurate and stable.
High-Quality Materials: Premium zirconia or hybrid prosthetics resist wear, staining, and fracture far better than acrylic alternatives.
Factors That Influence Longevity
Even the best dental implants can fail if certain factors aren’t optimized. Here’s what truly affects lifespan:
Surgical Expertise – Proper implant angulation and bone engagement are critical for long-term stability.
Material Choice – Cheaper acrylic or resin bridges tend to wear faster. Zirconia restorations can last decades.
Patient Health & Maintenance – Good daily hygiene, routine cleanings, and avoiding smoking are essential.
Technology Used – Newer digital workflows and guided placement reduce errors that shorten implant life.
What the Research Says
Studies show implant success rates of 95–98% at 10+ years, and many patients enjoy decades of function without replacement. Cases restored with premium zirconia and managed by experienced surgical-prosthetic teams show especially strong outcomes.
At The Dental Center Collective, our focus is on precision-engineered, long-lasting restorations — using digital planning, photogrammetry, and collaborative prosthodontic expertise for every case.
The longest follow-up of the All-on-4® treatment concept: Nobel Biocare Dental Implants
Implant dentistry is continually changing and Nobel Biocare has consistently provided dental implant solutions that are backed by scientific evidence. Nobel Biocare spends more in research and development than almost any other competitor in the industry.1 One recent study showed that, in the past 20 years, Nobel Biocare implants were evaluated in a greater number of research studies than products from most of its competitors. The All-on-4® treatment concept is a predictable treatment modality for full-arch rehabilitation with good results in the short, medium and long term.
Find more about this study in our recent article, “All-on-4® treatment concept: High rates of long-term clinical success”.
Real Results Across New England
We’ve seen patients from New Hampshire, Massachusetts, and Maine come to us after struggling with failing dentures or short-lived implant work done elsewhere.
When treatment is done right the first time — with proper planning, materials, and follow-up — the difference in comfort, function, and longevity is dramatic.
How to Make Your All-on-4 Last a Lifetime
Here’s how you can protect your investment:
Brush and floss daily using implant-safe tools.
Visit your implant dentist for cleanings every 4–6 months.
Wear a nightguard if you clench or grind your teeth.
Avoid smoking and heavy alcohol use, which impair healing.
Considering All-on-4 in New England?
If you’re ready for a smile that’s built to last, start with a comprehensive All-on-4 consultation at The Dental Center Collective. Our New England-based team specializes in advanced implant dentistry with long-term outcomes in mind.
📍 Serving patients from New Hampshire, Massachusetts, Maine, and beyond.
📞 Book your consultation today and take the first step toward a lifetime smile.
References
1. Sarkis-Onofre R, Marchini L, Spazzin AO, Santos MBFD. Randomized controlled trials in implant dentistry: assessment of the last 20 years of contribution and research network analysis. J Oral Implantol 2019;45(4):327-333.
Microplastics in Dentistry: What Patients Should Know
Discover how microplastics impact dental care, their potential health risks, and what patients can do to reduce exposure in everyday oral health routines.
How Microplastics Appear in Dentistry
Microplastics in dentistry can come from multiple sources, ranging from the products used at home to materials applied during dental procedures.
1. Toothpaste and Mouthwash
Some toothpastes, especially older formulas, contain tiny plastic beads—called microbeads—that help polish teeth. While these microbeads were designed for cosmetic purposes, they do not break down easily and can contribute to environmental pollution. Similarly, certain mouthwashes may contain microplastics as part of their formulations for texture or visual appeal.
2. Dental Materials
Dental procedures often use resin-based composites, sealants, and other plastic-containing materials. Over time, these materials can degrade slightly, potentially releasing microscopic plastic particles. While modern dental materials are highly durable and safe for patients, awareness of their composition is valuable for those seeking to minimize exposure.
3. Single-Use Plastics in Dental Offices
Dental practices rely on single-use plastics for safety and hygiene. Items like gloves, suction tips, protective barriers, and disposable cups are essential for infection control. However, when these plastics break down, they can generate microplastics. Even with strict dental waste management, some small particles may be released into the environment.
Are Microplastics Dangerous?
Research on microplastics is ongoing, and there is no definitive evidence yet that the levels encountered in dental care cause significant harm. However, scientists are studying potential long-term effects, including:
Inflammation: Microplastics may trigger low-level inflammatory responses in the body.
Gut health disruption: If ingested, microplastics could affect gut bacteria and overall digestive health.
Tissue accumulation: Some studies have found microplastics in human tissues, though the clinical impact remains unclear.
For patients, it’s important to balance awareness with perspective. While microplastics are a valid concern, dental care is essential for oral and overall health, and avoiding necessary treatments is not recommended.
How Patients Can Reduce Exposure to Microplastics
Fortunately, there are practical steps patients can take to minimize microplastic exposure without compromising dental health.
1. Choose Microplastic-Free Oral Care Products
Look for toothpaste and mouthwash labeled “microplastic-free” or “no plastic microbeads.” Many modern brands now offer safe, biodegradable alternatives. These products are just as effective for cleaning teeth and maintaining oral health.
2. Discuss Dental Materials With Your Dentist
When getting fillings, crowns, or sealants, ask your dentist about the materials being used. Some resin-based composites may contain microplastics, while others are formulated with safer, more environmentally friendly alternatives. Open communication allows patients to make informed decisions about their dental care.
3. Support Eco-Friendly Dental Practices
Many dental offices, like The Dental Center, are adopting sustainable practices, such as:
Reducing single-use plastics where safe and possible
Using biodegradable or recyclable packaging
Implementing advanced sterilization and waste management systems
Choosing a practice that prioritizes sustainability can reduce your environmental footprint and minimize exposure to microplastics.
4. Proper Disposal of Oral Care Products
Even at home, disposal matters. Microplastics from toothpaste, floss containers, and other oral care items can enter waterways if not discarded properly. Opting for recyclable packaging and disposing of products responsibly helps reduce environmental contamination.
Why Microplastics Matter for Overall Health
While microplastics in dentistry are just one piece of the puzzle, their presence highlights a broader issue of plastic exposure in daily life. Reducing microplastics is not just about oral health—it’s about overall health and environmental responsibility.
Studies have suggested links between microplastic exposure and:
Respiratory issues if airborne particles are inhaled
Digestive system disturbances when ingested through food, water, or dental products
Cellular stress and inflammation in lab studies
Dental patients can see their choices as part of a larger effort to protect personal health and the planet.
The Future of Dentistry and Microplastics
Dental research is actively exploring safer, more sustainable alternatives to traditional plastic materials. Innovations include:
Biodegradable composites for fillings and sealants
Plastic-free impression materials for crowns, bridges, and dentures
Reduced reliance on single-use plastics in clinics while maintaining strict hygiene standards
These advances aim to minimize microplastic exposure without compromising patient safety or treatment outcomes.
Key Takeaways for Patients
Microplastics are tiny plastic particles that can appear in toothpaste, dental materials, and single-use items in dental offices.
The levels of microplastics in dental care are generally low, but reducing exposure is still beneficial.
Patients can choose microplastic-free oral care products, discuss materials with their dentist, and support eco-conscious practices.
Responsible disposal of dental and oral care products helps protect the environment and reduce microplastic pollution.
Ongoing research in dentistry is paving the way for safer, more sustainable materials.
Final Thoughts
While microplastics in dentistry are a growing concern, being informed empowers patients to make choices that protect their health and the environment. By asking questions, selecting sustainable products, and supporting environmentally conscious dental practices, patients can reduce their exposure without compromising the quality of their dental care.
Dental health is essential, and small adjustments can make a big difference in minimizing microplastic exposure. Staying aware and proactive allows patients to enjoy a healthy smile while contributing to a cleaner, safer world.
The Impact of Periodontal Disease on Cardiovascular Health: Understanding the Connection
Periodontal disease affects a large number of adults over 55, with 60–70% showing signs of gum disease, from mild gingivitis to advanced periodontitis. Age-related factors, systemic conditions like diabetes, and long-term plaque buildup contribute to this increased risk. Maintaining regular dental check-ups and periodontal care is essential for seniors to protect oral health, prevent tooth loss, and reduce potential systemic complications associated with chronic gum inflammation.
Periodontal disease, commonly known as gum disease, is a prevalent condition affecting millions worldwide. While its effects are often confined to oral health, emerging research suggests a significant link between periodontal disease and cardiovascular health. This connection underscores the importance of maintaining good oral hygiene not only for a healthy smile but also for a healthy heart.
What Is Periodontal Disease?
Periodontal disease encompasses a range of inflammatory conditions affecting the tissues surrounding and supporting the teeth. It typically begins with gingivitis, characterized by gum inflammation and bleeding. If left untreated, it can progress to periodontitis, leading to gum recession, tooth mobility, and potential tooth loss.
Periodontal disease becomes increasingly common with age, affecting a significant proportion of adults over 55. Research indicates that approximately 60–70% of individuals in this age group show signs of some form of periodontal disease, ranging from mild gingivitis to advanced periodontitis. Age-related factors such as reduced immune response, systemic health conditions (like diabetes and cardiovascular disease), and cumulative oral plaque exposure contribute to this higher prevalence. This underscores the importance of regular dental check-ups and periodontal maintenance for older adults to prevent tooth loss, maintain oral function, and reduce potential systemic health risks associated with chronic gum inflammation. (Cender for Disease Control and Prevention, 2023)
The Link Between Oral and Heart Health
Recent studies have illuminated the association between periodontal disease and cardiovascular disease (CVD). Individuals with periodontal disease are at a heightened risk of developing heart-related conditions, including heart attacks, strokes, and peripheral artery disease.
One notable study published in the European Heart Journal found that treating severe gum disease could slow the thickening of the carotid arteries, a known marker for cardiovascular disease. Participants who received intensive dental treatment exhibited reduced arterial thickening and improved blood vessel function over two years.
Mechanisms Linking Periodontal Disease to Cardiovascular Health
The connection between oral health and heart health is believed to involve several mechanisms:
Bacterial Translocation: Oral bacteria can enter the bloodstream through inflamed gum tissues. These bacteria may contribute to the formation of arterial plaque, leading to atherosclerosis.
Systemic Inflammation: Periodontal disease triggers an inflammatory response that can elevate levels of inflammatory markers. Chronic inflammation is a known risk factor for cardiovascular events.
Oxidative Stress: The presence of periodontal pathogens can damage blood vessels and promote the development of cardiovascular diseases.
Evidence from Research
A systematic review and meta-analysis revealed a significant association between periodontal disease and cardiovascular diseases, including myocardial infarction, stroke, and peripheral artery disease. The review indicated that individuals with periodontal disease had a 20% higher risk of cardiovascular events compared to those without.
Further studies have shown that periodontal treatment can lead to improvements in cardiovascular health markers. For instance, non-surgical periodontal therapy has been associated with reductions in blood pressure and improvements in endothelial function, which is crucial for vascular health.
Preventive Measures
Maintaining optimal oral hygiene is essential for preventing periodontal disease and its potential impact on cardiovascular health:
Regular Brushing and Flossing: Brush teeth at least twice daily and floss once a day to remove plaque and prevent gum inflammation.
Regular Dental Check-ups: Visit a dentist regularly for professional cleanings and early detection of periodontal issues.
Healthy Lifestyle Choices: Avoid smoking, maintain a balanced diet, and manage stress to reduce the risk of both periodontal and cardiovascular diseases.
Conclusion
The growing body of evidence highlights the significant impact of periodontal disease on cardiovascular health. By understanding this connection and adopting preventive measures, individuals can safeguard both their oral and heart health. Regular dental care and a healthy lifestyle are pivotal in reducing the risk of cardiovascular events associated with periodontal disease.
Replacing Missing Teeth: Your Guide to Restoring Your Smile
Missing teeth can affect your health, confidence, and quality of life. Discover the best tooth replacement options—like dental implants, bridges, and dentures—and learn which treatment is right for you. Explore how modern dentistry can restore your smile with long-lasting results.
Tooth loss is more common than you might think. Whether due to decay, gum disease, trauma, or aging, millions of Americans are missing at least one tooth—and many are missing several. Fortunately, modern dentistry offers effective and lasting solutions to replace missing teeth, restore your smile, and improve your oral health.
In this guide, we'll explore the best tooth replacement options available, their benefits, how they work, and how to choose the right solution for your unique needs.
Why Replace Missing Teeth?
Before diving into your treatment options, it’s important to understand why replacing missing teeth matters—not just cosmetically, but for your overall health.
Missing teeth can lead to:
Bone loss in the jaw due to lack of stimulation
Shifting of surrounding teeth, leading to bite problems
Speech and chewing difficulties
Premature facial aging due to loss of facial structure
Lowered self-esteem from gaps or altered smile
Replacing missing teeth isn’t just about aesthetics—it’s about restoring function, confidence, and preventing long-term oral health issues.
Top Tooth Replacement Options
There are several proven options to replace missing teeth. Each offers unique benefits depending on your goals, budget, and overall dental health.
1. Dental Implants: The Gold Standard
Best for: Long-term, natural-feeling tooth replacement
Dental implants are widely considered the most effective and permanent solution for missing teeth. An implant is a small titanium post that is surgically placed into your jawbone to act as an artificial root. A crown, bridge, or denture is then attached to complete the restoration.
Key Benefits:
Mimics natural tooth structure
Prevents bone loss and preserves facial structure
Doesn’t affect neighboring teeth
Long-lasting (often a lifetime with proper care)
High success rate (over 95%)
Ideal Candidates:
You should have healthy gums, adequate jawbone density, and be in overall good health. Bone grafting may be needed if bone loss has occurred.
Types of Implants:
Single-Tooth Implant for one missing tooth
Implant Bridge for several missing teeth
All-on-4/All-on-X for full-arch restoration using just 4–6 implants
2. Fixed Dental Bridge
Best for: Replacing one or several adjacent teeth
A dental bridge literally “bridges” the gap left by missing teeth. It uses the surrounding teeth as anchors (or abutments) and places an artificial tooth (pontic) in the gap.
Key Benefits:
Restores chewing function and appearance
Faster treatment than implants (no surgery)
Less expensive than implants
Drawbacks:
Requires grinding down healthy teeth to support the bridge
Doesn’t prevent bone loss
May need replacement every 5–15 years
3. Removable Partial Dentures
Best for: Replacing several missing teeth in different areas of the mouth, when implants are not possible
Partial dentures consist of replacement teeth attached to a gum-colored plastic base, often supported by a metal framework that clips onto existing teeth.
Key Benefits:
Affordable
Non-invasive
Easy to remove and clean
Drawbacks:
Less stable than implants or bridges
May affect speech or comfort
Requires frequent adjustments
4. Full Dentures
Best for: Complete tooth loss in the upper or lower jaw
Traditional full dentures sit on top of the gums and are custom made to fit your mouth.
Key Benefits:
Affordable full-mouth solution
Non-surgical
Fast turnaround
Drawbacks:
Can slip or move while eating or speaking
May require adhesives
Bone loss continues underneath
Upgrade Option: Implant-Supported Dentures
Also known as overdentures, these snap onto dental implants for improved stability and comfort. They prevent bone loss and feel more like natural teeth.
How to Choose the Right Tooth Replacement Option
Several factors affect your treatment plan:
1. Number of Missing Teeth
One or two missing teeth: dental implants or bridges
Several missing teeth: implant bridge, partial dentures, or overdentures
Full arch missing: All-on-4, All-on-X, or full dentures
2. Bone Health
Implants require healthy jawbone. Bone grafting may be needed.
Dentures and bridges don’t require bone support.
3. Budget
Dentures and bridges have lower upfront costs.
Implants are more expensive initially but may be more cost-effective long term.
4. Lifestyle and Preferences
Implants offer the closest feel to natural teeth.
Dentures may require more maintenance and lifestyle adjustments.
5. Health Conditions
Chronic health issues like diabetes or smoking can affect implant success.
Non-surgical options may be preferable in these cases.
The Tooth Replacement Process: What to Expect
Your smile journey will involve several key steps:
1. Comprehensive Dental Evaluation
Your dentist or prosthodontist will assess your oral health, take digital scans or X-rays, and recommend the best treatment plan.
2. Treatment Planning
This includes mapping out tooth replacements, scheduling surgery (if needed), and preparing any supporting structures.
3. Procedure
Depending on the treatment, you may undergo:
Implant surgery (with a healing period)
Tooth preparation for bridges
Impressions for dentures or bridges
4. Restoration Placement
Final crowns, bridges, or dentures are custom fabricated and placed.
5. Follow-Up and Maintenance
Regular cleanings, exams, and proper home care ensure long-term success.
Long-Term Care for Your Tooth Replacement
No matter which treatment you choose, good oral hygiene is essential.
Brush and floss daily (or as directed)
Use a water flosser for bridges or implants
Clean dentures thoroughly each day
Visit your dentist regularly for cleanings and exams
Replacing Missing Teeth in New Hampshire?
Visit Our Specialty Dental Clinic
At The Dental Center Collective, we specialize in full-mouth rehabilitation, dental implants, and premium tooth replacement solutions in New Hampshire. Our patient-focused, luxury clinic experience ensures comfort, expertise, and lasting results.
Whether you're missing one tooth or need a complete restoration, we’re here to guide you every step of the way. Schedule a consultation today and take the first step toward a confident, healthy smile.
Frequently Asked Questions
Q: Is it OK to not replace a missing tooth?
A: While it’s possible to live without one, missing teeth can cause long-term damage to your bite, bone, and overall health. Replacing them is highly recommended.
Q: Are dental implants painful?
A: Most patients report minimal discomfort related to pressure or vibration during the procedure. The process is typically done under local anesthesia and healing is well-tolerated.
Q: How long do tooth replacements last?
A: Implants can last a lifetime. Bridges and dentures typically last 5–15 years with proper care. Best practices recommend replacement of removable prostheses every 5 years.
Why You Shouldn’t Shop for Dental Implants by Price Alone
Don't choose dental implants based on price alone. Learn the hidden risks of low-cost offers and what to look for in a quality implant provider.
When it comes to your smile, few things are more life-changing than dental implants. They restore your ability to eat, speak, and smile with confidence. But as patients begin their research, one question often rises to the top: “How much do dental implants cost?”
It’s a valid question—but focusing solely on price can be a costly mistake. Like any long-term investment in your health and well-being, dental implants should be judged by more than just the price tag.
In this post, we’ll explain why shopping for dental implants by price alone is risky, what hidden costs you should look out for, and what truly makes one provider more valuable than another.
The Temptation of Low-Cost Dental Implants
A quick Google search will show wide variations in dental implant pricing. You might see one office offering implants “starting at $999” while others quote $20,000 or more for full-mouth solutions like All-on-4. So what gives?
The truth is, not all dental implants—or implant providers—are created equal. Cheap implants may seem appealing up front, but they often come with trade-offs that cost you more in the long run.
10 Reasons Not to Choose Dental Implants Based on Price Alone
1. Not All Prices Include the Same Services
Many low-price ads are “bait and switch” offers. They may only include the implant post—not the abutment, crown, bone grafting, imaging, or anesthesia. Once everything is added up, the price often matches or exceeds what reputable offices charge upfront.
Ask: Does the quote include the full procedure—surgery, crown, and follow-up?
2. Materials Matter
Dental implants vary in quality, just like cars or phones. Cheaper providers may use low-cost implant brands made from subpar titanium alloys or poor design. These can:
Integrate poorly with bone
Fail prematurely
Be harder to restore later if they break
We use premium, proven implant systems with long-term clinical success rates.
3. Experience of the Surgical Team
Would you trust a heart surgery to the cheapest surgeon in town?
Implant placement is a highly specialized procedure. The experience of your provider directly impacts your outcome. Improper implant placement can result in:
Nerve damage
Implant failure
Bite misalignment
A smile that doesn’t look natural
We’ve restored hundreds of smiles with a surgical and prosthetic team that works together under one roof—ensuring safety, precision, and beautiful results.
4. Technology and Diagnostics
Quality implant centers invest in 3D CBCT imaging, guided surgery, digital design tools, and in-house labs. These technologies reduce guesswork and improve accuracy.
Cheaper offices may skip these steps to cut costs—leading to increased risk of failure, improper placement, or the need for re-treatment later.
5. One Day, but Done Right
You may have seen ads promoting “teeth in a day” or same-day implants. While it’s true that procedures like All-on-4 can restore your smile in one day, not all “one-day” providers offer:
Proper pre-surgical planning
A customized prosthetic (instead of a generic one)
Follow-up care and adjustments
Fast doesn’t mean careless. We ensure your smile is not only delivered quickly—but safely and beautifully.
6. Long-Term Results vs. Short-Term Fixes
Dental implants are meant to last decades, if not a lifetime. Choosing a provider based on the lowest quote may save you today but cost you much more in repairs or replacement later.
It’s like buying a cheap roof—it may look fine now, but you’ll pay the price when it leaks in five years.
7. Hidden Costs of Travel Dentistry
Some patients consider traveling to other states—or even other countries—for cheaper implants. But:
What happens if something goes wrong?
Who handles the follow-up?
What if you have complications a month later?
Many patients who go the “cheap travel” route end up back home needing repairs—at full cost and with more challenges.
8. Lack of Warranty or Follow-Up Care
Reputable implant providers offer warranties and ongoing maintenance. Many low-cost providers:
Rush through the process
Disappear after the procedure
Don’t offer follow-up appointments or cleanings
Your implant journey doesn’t end after surgery—it’s a lifelong investment, and you deserve a partner who’s there for you long-term.
9. Your Smile Aesthetics Are Worth It
Implants don’t just replace teeth—they rebuild your smile, confidence, and self-image. Choosing a provider who understands facial harmony, natural aesthetics, and bite alignment is crucial.
Cheaper providers may not customize your smile to your face, age, or personality. The result? Teeth that look fake or feel wrong in your mouth.
10. You're Not Just Buying Implants—You're Buying Trust
When you choose a dental implant provider, you’re not buying a screw and a crown. You’re buying:
Expertise
Peace of mind
Personalized care
A team that takes time to understand your goals
Choosing based on trust and proven results will always beat chasing the lowest number.
What Should You Look for Instead?
When comparing implant providers, consider these questions:
Is the quote all-inclusive?
How many implants have they placed?
Do they use 3D imaging and guided surgery?
Will I see the same team throughout the process?
Do they offer in-house financing or warranties?
Are before-and-after photos and patient reviews available?
The best implant centers are transparent, experienced, and focused on your outcome—not just the transaction.
Final Thoughts: Value Over Price, Always
Dental implants are one of the most powerful investments you can make in your health. While cost is important, it should never be the only factor.
A lower price today could mean:
A shorter lifespan for your implants
Additional surgeries later
A smile that doesn’t function or feel right
Regret
Instead, choose a provider who focuses on quality, outcomes, and personalized care.
Ready to Explore Your Options?
Schedule a consultation, where you can:
Get a clear, all-inclusive quote
Review your smile goals
Understand your candidacy
Explore flexible financing plans
Let us help you invest wisely in your future smile.